These videos give an overview of the various Home and Community-Based Services (HCBS) available in New Jersey for providers who want to learn how to start or operate an HCBS agency in the state. Each video explains the purpose of the service, provider requirements, licensing process, and how the program functions. Use these videos to better understand the responsibilities, standards, and steps involved in becoming or working with approved HCBS providers in New Jersey. Explore each section to find the service that best matches your goals or area of interest.
Respite Care
RESPITE CARE SERVICES PROVIDER IN NEW JERSEY
SUPPORTING CAREGIVERS AND PROMOTING WELL-BEING THROUGH TEMPORARY RELIEF SERVICES
Respite Care Services in New Jersey provide temporary relief for family caregivers of individuals with disabilities, chronic illnesses, or age-related conditions. These services allow primary caregivers to rest, attend to personal matters, or recover from caregiver fatigue while ensuring the participant’s safety and well-being. Respite Care Services are authorized under New Jersey Medicaid Home and Community-Based Services (HCBS) Waiver programs.
1. GOVERNING AGENCIES
Agency: New Jersey Department of Human Services (DHS)
Role: Administers Medicaid waiver funding for Respite Care Services and manages provider enrollment, service authorization, and reimbursement.
Agency: Division of Developmental Disabilities (DDD)
Role: Ensures quality standards, service delivery, and compliance for Respite Care Services under HCBS waiver programs.
Agency: Centers for Medicare & Medicaid Services (CMS)
Role: Provides federal oversight ensuring Medicaid-funded Respite Care Services meet HCBS quality, person-centered planning, and participant protection standards.
2. RESPITE CARE SERVICES OVERVIEW
Respite Care Services offer planned or emergency relief for unpaid caregivers while ensuring participants receive appropriate supervision, personal care, and support services.
Approved providers may deliver:
In-Home Respite Services: Care provided in the participant’s residence.
Facility-Based Respite Care: Temporary care in licensed community settings.
Day Respite: Supervision and support during daytime hours.
Overnight or Weekend Respite: Extended care to accommodate caregiver breaks.
Personal Care Assistance: Help with Activities of Daily Living (ADLs) such as bathing, grooming, feeding, mobility, and toileting.
Medication Reminders: Non-skilled assistance with medication schedules.
Social Engagement: Facilitating recreational or therapeutic activities based on the participant’s interests and care plan.
All respite care must align with the participant’s Individualized Service Plan (ISP) and reflect their health and safety needs.
3. LICENSING & PROVIDER APPROVAL REQUIREMENTS
Prerequisites:
Register the business entity with the New Jersey Division of Revenue and Enterprise Services.
Obtain EIN from the IRS and NPI (Type 2).
Enroll as a Medicaid Waiver Respite Care provider through the New Jersey Medicaid Provider Enrollment Portal.
Obtain facility licensure (if providing facility-based respite) from DHS or other relevant agencies.
Maintain general liability and professional liability insurance.
Develop comprehensive policies for participant intake, caregiver communication, incident reporting, and emergency procedures.
Ensure all direct care staff meet background screening, health screenings, and training requirements.
4. NEW JERSEY PROVIDER ENROLLMENT PROCESS
Initial Interest and Application:
Submit Provider Enrollment Application through the New Jersey Medicaid Provider Enrollment Portal for Respite Care Services under appropriate HCBS waivers.
Application and Documentation Submission:
Submit Articles of Incorporation, proof of EIN/NPI, liability insurance certificates, staff credentialing documentation, and service policies.
Program Readiness Review:
DHS and DDD review provider readiness, including staff qualifications, care and supervision protocols, participant safety plans, and documentation systems.
Approval & Medicaid Enrollment:
Upon approval, providers are authorized to bill Medicaid for In-Home and/or Facility-Based Respite Services using assigned billing codes.
5. REQUIRED DOCUMENTATION
Articles of Incorporation or Business License (New Jersey Division of Revenue)
IRS EIN confirmation
NPI confirmation
Facility License (for facility-based respite providers)
Proof of general and professional liability insurance
Respite Care Services Policy & Procedure Manual including:
Participant intake, care planning, and service scheduling procedures
Health and safety monitoring, medication reminders, and supervision protocols
Emergency preparedness, abuse prevention, and critical incident reporting policies
Participant rights, HIPAA confidentiality procedures, and grievance handling
Staff credentialing, background checks, first aid/CPR certification documentation
Medicaid billing, service tracking, and audit readiness procedures
6. STAFFING REQUIREMENTS
Role: Respite Services Program Director
Requirements: Bachelor’s degree in human services, healthcare, or related field; supervisory experience preferred.
Role: Respite Care Workers
Requirements: High school diploma or GED; CPR/First Aid certification; completion of respite-specific or direct care training; background screening and health clearance.
All staff must complete:
Safety and emergency preparedness training
HIPAA compliance and participant rights education
Abuse prevention and exploitation awareness training
Infection control and health monitoring training
Annual competency evaluations and continuing education
7. MEDICAID WAIVER PROGRAMS
Respite Care Services are available under the following New Jersey Medicaid Waivers:
Community Care Program for the Elderly and Disabled (CCPED)
Supports Program Waiver
Acquired Brain Injury (ABI) Waiver
Personal Care Assistant (PCA) Waiver
Home and Community-Based Services (HCBS) Waiver
Services may include:
In-home or facility-based supervision and care
Temporary support allowing unpaid caregivers to attend to personal needs
Assistance with basic ADLs and wellness monitoring during respite periods
Crisis respite services when caregiver availability is compromised
8. TIMELINE TO LAUNCH
Phase: Business Formation and Compliance Preparation
Timeline: 1–2 months
Phase: Staff Hiring, Credentialing, and Program Development
Timeline: 2–3 months
Phase: New Jersey Medicaid Provider Enrollment and Readiness Review
Timeline: 60–90 days
Phase: Medicaid Billing Setup and Respite Care Service Launch
Timeline: 30–45 days
9. CONTACT INFORMATION
New Jersey Department of Human Services (DHS)
Website: https://www.state.nj.us/humanservices/
Division of Developmental Disabilities (DDD)
Website: https://www.state.nj.us/humanservices/ddd/
New Jersey Medicaid Provider Enrollment Portal
Website: https://www.njmmis.com/
Centers for Medicare & Medicaid Services (CMS)
Website: https://www.cms.gov/
WAIVER CONSULTING GROUP’S START-UP ASSISTANCE SERVICE — NEW JERSEY RESPITE CARE SERVICES PROVIDER
WCG supports agencies in launching Medicaid-compliant Respite Care Services in New Jersey, offering:
Scope of Work:
Business registration, Medicaid enrollment, and facility licensure support
Policy manual development for respite care planning and caregiver communication
Staff credentialing templates, participant intake forms, and emergency planning templates
Medicaid billing system setup and audit-ready claims management
Branding, website development, and caregiver engagement strategies
Quality assurance systems for incident reporting, service tracking, and compliance monitoring

Residential Support
RESIDENTIAL SUPPORT SERVICES PROVIDER IN NEW JERSEY
SUPPORTING INDEPENDENT LIVING AND COMMUNITY INTEGRATION THROUGH RESIDENTIAL CARE
Residential Support Services in New Jersey provide individuals with disabilities, chronic conditions, or age-related challenges with safe and supportive living environments. These services aim to promote independence, personal growth, and community integration. Residential Support Services are authorized under New Jersey Medicaid Home and Community-Based Services (HCBS) Waiver programs.
1. GOVERNING AGENCIES
Agency: New Jersey Department of Human Services (DHS)
Role: Administers Medicaid waiver funding for Residential Support Services and manages provider enrollment, service authorization, and reimbursement.
Agency: Division of Developmental Disabilities (DDD)
Role: Ensures quality standards, service delivery, and compliance for Residential Support Services under HCBS waiver programs.
Agency: Centers for Medicare & Medicaid Services (CMS)
Role: Provides federal oversight ensuring Medicaid-funded Residential Support Services meet HCBS quality, person-centered planning, and participant protection standards.
2. RESIDENTIAL SUPPORT SERVICES OVERVIEW
Residential Support Services provide safe, structured living environments for individuals who need assistance with daily living and community integration.
Approved providers may deliver:
24/7 Residential Care: Supervised living arrangements with staff support.
Assistance with Activities of Daily Living (ADLs): Personal care, mobility support, and health monitoring.
Skill Development: Teaching daily living skills like cooking, cleaning, and budgeting.
Community Engagement: Facilitating participation in social, recreational, and educational activities.
Health and Safety Monitoring: Ensuring a safe and supportive living environment.
Behavioral Support: Assistance with managing challenging behaviors.
Emergency and Crisis Intervention: Immediate support during emergencies.
Personalized Care Plans: Developing individualized plans tailored to the participant’s needs.
All services are delivered according to the Individualized Service Plan (ISP) to meet the participant’s residential and support needs.
3. LICENSING & PROVIDER APPROVAL REQUIREMENTS
Prerequisites:
Register the business entity with the New Jersey Division of Revenue and Enterprise Services.
Obtain EIN from the IRS and NPI (Type 2).
Enroll as a Medicaid Waiver Residential Support provider via the New Jersey Medicaid Provider Enrollment Portal.
Obtain residential facility licensure from DHS, DDD, or the New Jersey Department of Community Affairs (DCA).
Maintain general liability and professional liability insurance.
Develop policies for residential care, safety protocols, and staff training.
Ensure staff meet background checks, health screenings, and residential care training requirements.
4. NEW JERSEY PROVIDER ENROLLMENT PROCESS
Initial Interest and Application:
Complete the Provider Enrollment Application through the New Jersey Medicaid Provider Enrollment Portal for Residential Support Services under HCBS waivers.
Application and Documentation Submission:
Submit Articles of Incorporation, proof of EIN/NPI, residential facility licenses, insurance certificates, and policy manuals.
Program Readiness Review:
DHS and DDD evaluate provider readiness, including facility safety, staff qualifications, and care protocols.
Approval & Medicaid Enrollment:
Upon approval, providers are authorized to bill Medicaid for Residential Support Services using designated billing codes.
5. REQUIRED DOCUMENTATION
Articles of Incorporation or Business License (New Jersey Division of Revenue)
IRS EIN confirmation
NPI confirmation
Residential Facility License (if applicable)
Proof of general and professional liability insurance
Residential Support Services Policy & Procedure Manual including:
Participant intake, assessment, and individualized care planning procedures
Health and safety monitoring, medication management, and emergency preparedness
Staff credentialing, background checks, and ongoing training records
Documentation standards for residential care tracking and Medicaid billing
HIPAA compliance, participant rights, and grievance handling
Safety protocols, emergency response, and crisis intervention measures
Quality assurance and compliance monitoring
6. STAFFING REQUIREMENTS
Role: Residential Support Program Director
Requirements: Bachelor’s or Master’s degree in human services, social work, or healthcare administration; supervisory experience preferred.
Role: Direct Support Professionals (DSPs)
Requirements: High school diploma or GED; CPR/First Aid certification; training in personal care and ADL support; background clearance.
Role: Residential Care Supervisors
Requirements: Experience in residential care management; supervisory experience; background clearance.
Role: Behavioral Support Specialists (if applicable)
Requirements: Certification in behavioral health support or applied behavior analysis (ABA); background clearance.
All staff must complete:
Training in residential safety and emergency protocols
HIPAA compliance and participant rights education
Annual competency evaluations and ongoing professional development
Behavioral intervention and crisis management training
Infection control and wellness monitoring education
7. MEDICAID WAIVER PROGRAMS
Residential Support Services are available under the following New Jersey Medicaid Waivers:
Community Care Program for the Elderly and Disabled (CCPED)
Supports Program Waiver
Acquired Brain Injury (ABI) Waiver
Personal Care Assistant (PCA) Waiver
Home and Community-Based Services (HCBS) Waiver
Services may include:
24-hour supervised residential care
Assistance with personal care and ADLs
Community participation and social skill development
Health and wellness monitoring
Behavioral support and crisis intervention
8. TIMELINE TO LAUNCH
Phase: Business Formation and Compliance Preparation
Timeline: 1–2 months
Phase: Facility Licensing and Compliance Documentation
Timeline: 2–3 months
Phase: Staff Hiring, Credentialing, and Training
Timeline: 2–3 months
Phase: New Jersey Medicaid Provider Enrollment and Readiness Review
Timeline: 60–90 days
Phase: Medicaid Billing Setup and Residential Support Service Launch
Timeline: 30–45 days
9. CONTACT INFORMATION
New Jersey Department of Human Services (DHS)
Website: https://www.state.nj.us/humanservices/
Division of Developmental Disabilities (DDD)
Website: https://www.state.nj.us/humanservices/ddd/
New Jersey Department of Community Affairs (DCA)
Website: https://www.nj.gov/dca/
New Jersey Medicaid Provider Enrollment Portal
Website: https://www.njmmis.com/
Centers for Medicare & Medicaid Services (CMS)
Website: https://www.cms.gov/
WAIVER CONSULTING GROUP’S START-UP ASSISTANCE SERVICE — NEW JERSEY RESIDENTIAL SUPPORT SERVICES PROVIDER
WCG supports agencies in launching Medicaid-compliant Residential Support Services in New Jersey, offering:
Scope of Work:
Business registration, Medicaid enrollment, and facility licensure support
Policy manual development for residential care and community integration
Staff credentialing, training program templates, and documentation guidance
Medicaid billing setup and audit-prepared financial management
Branding, website development, and community outreach strategies
Quality assurance systems for residential care safety and compliance
Collaboration with healthcare and community organizations

Supported Employment
SUPPORTED EMPLOYMENT SERVICES PROVIDER IN NEW JERSEY
EMPOWERING INDIVIDUALS THROUGH VOCATIONAL SUPPORT AND COMMUNITY INTEGRATION
Supported Employment Services in New Jersey assist individuals with disabilities, chronic conditions, or other barriers to employment by providing vocational training, job placement, and on-the-job support. These services help individuals gain and maintain meaningful employment, fostering independence and community inclusion. Supported Employment Services are authorized under New Jersey Medicaid Home and Community-Based Services (HCBS) Waiver programs.
1. GOVERNING AGENCIES
Agency: New Jersey Department of Human Services (DHS)
Role: Administers Medicaid waiver funding for Supported Employment Services and manages provider enrollment, service authorization, and reimbursement.
Agency: Division of Vocational Rehabilitation Services (DVRS)
Role: Facilitates access to vocational support and employment services for individuals with disabilities.
Agency: Division of Developmental Disabilities (DDD)
Role: Ensures quality standards, service delivery, and compliance for Supported Employment Services under HCBS waiver programs.
Agency: Centers for Medicare & Medicaid Services (CMS)
Role: Provides federal oversight ensuring Medicaid-funded Supported Employment Services meet HCBS quality, person-centered planning, and participant protection standards.
2. SUPPORTED EMPLOYMENT SERVICES OVERVIEW
Supported Employment Services are designed to help individuals find, secure, and retain competitive employment in the community.
Approved providers may deliver:
Vocational Assessment: Identifying skills, interests, and employment goals.
Job Development and Placement: Assisting individuals in finding suitable job opportunities.
Job Coaching: Providing on-site support and skill development.
Job Retention Support: Monitoring progress and addressing workplace challenges.
Career Counseling: Helping individuals develop long-term vocational goals.
Soft Skills Training: Improving communication, teamwork, and problem-solving skills.
Employer Engagement: Educating employers on accommodating individuals with disabilities.
Follow-Up and Retention Monitoring: Ongoing support to maintain job stability.
All services are delivered according to the Individualized Service Plan (ISP) to meet the participant’s vocational goals and support needs.
3. LICENSING & PROVIDER APPROVAL REQUIREMENTS
Prerequisites:
Register the business entity with the New Jersey Division of Revenue and Enterprise Services.
Obtain EIN from the IRS and NPI (Type 2).
Enroll as a Medicaid Waiver Supported Employment provider via the New Jersey Medicaid Provider Enrollment Portal.
Obtain necessary certifications for vocational support and job coaching.
Maintain general liability and professional liability insurance.
Develop policies for job placement, workplace safety, and support coordination.
Ensure staff meet background checks, health screenings, and vocational training requirements.
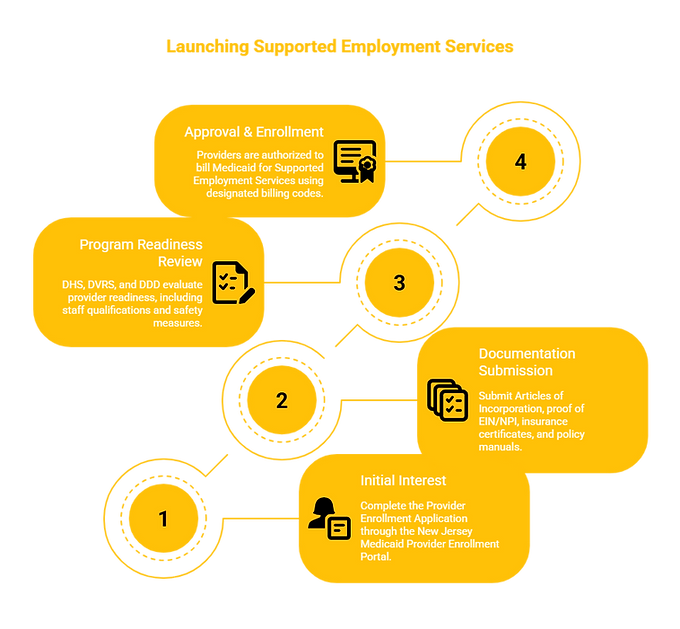
4. NEW JERSEY PROVIDER ENROLLMENT PROCESS
Initial Interest and Application:
Complete the Provider Enrollment Application through the New Jersey Medicaid Provider Enrollment Portal for Supported Employment Services under HCBS waivers.
Application and Documentation Submission:
Submit Articles of Incorporation, proof of EIN/NPI, insurance certificates, vocational training certifications, and policy manuals.
Program Readiness Review:
DHS, DVRS, and DDD evaluate provider readiness, including staff qualifications, vocational support protocols, and workplace safety measures.
Approval & Medicaid Enrollment:
Upon approval, providers are authorized to bill Medicaid for Supported Employment Services using designated billing codes.
5. REQUIRED DOCUMENTATION
Articles of Incorporation or Business License (New Jersey Division of Revenue)
IRS EIN confirmation
NPI confirmation
Proof of general and professional liability insurance
Supported Employment Services Policy & Procedure Manual including:
Vocational assessment, job placement, and coaching procedures
Staff credentialing, background checks, and ongoing training records
Documentation standards for service tracking and Medicaid billing
HIPAA compliance, participant rights, and grievance handling
Safety protocols for workplace environments and community-based work sites
Follow-up and retention support procedures
Quality assurance and compliance monitoring
6. STAFFING REQUIREMENTS
Role: Supported Employment Program Director
Requirements: Bachelor’s degree in vocational rehabilitation, social work, or related field; supervisory experience in employment services.
Role: Job Coaches
Requirements: Experience in vocational support or rehabilitation; training in job coaching and support strategies; background clearance.
Role: Vocational Counselors
Requirements: Certification in vocational rehabilitation or employment support; experience in career counseling; background clearance.
Role: Employment Specialists
Requirements: Experience in job development and placement; training in community-based employment support; background clearance.
All staff must complete:
Training in job coaching, soft skills development, and client safety
HIPAA compliance and participant rights education
Annual competency evaluations and professional development
Ongoing training in community employment support and job retention strategies
7. MEDICAID WAIVER PROGRAMS
Supported Employment Services are available under the following New Jersey Medicaid Waivers:
Community Care Program for the Elderly and Disabled (CCPED)
Supports Program Waiver
Acquired Brain Injury (ABI) Waiver
Personal Care Assistant (PCA) Waiver
Home and Community-Based Services (HCBS) Waiver
Services may include:
Job development and placement assistance
On-the-job training and coaching
Employment retention and follow-up support
Soft skills training for workplace success
Employer engagement and education
8. TIMELINE TO LAUNCH
Phase: Business Formation and Compliance Preparation
Timeline: 1–2 months
Phase: Staff Hiring, Credentialing, and Program Development
Timeline: 2–3 months
Phase: New Jersey Medicaid Provider Enrollment and Readiness Review
Timeline: 60–90 days
Phase: Medicaid Billing Setup and Supported Employment Service Launch
Timeline: 30–45 days
9. CONTACT INFORMATION
New Jersey Department of Human Services (DHS)
Website: https://www.state.nj.us/humanservices/
Division of Vocational Rehabilitation Services (DVRS)
Website: https://www.state.nj.us/humanservices/dvrs/
Division of Developmental Disabilities (DDD)
Website: https://www.state.nj.us/humanservices/ddd/
New Jersey Medicaid Provider Enrollment Portal
Website: https://www.njmmis.com/
Centers for Medicare & Medicaid Services (CMS)
Website: https://www.cms.gov/
WAIVER CONSULTING GROUP’S START-UP ASSISTANCE SERVICE — NEW JERSEY SUPPORTED EMPLOYMENT SERVICES PROVIDER
WCG supports agencies in launching Medicaid-compliant Supported Employment Services in New Jersey, offering:
Scope of Work:
Business registration, Medicaid enrollment, and licensing assistance
Policy manual development for vocational support and job coaching
Staff credentialing, training program templates, and compliance documentation
Medicaid billing setup and audit-prepared financial management
Branding, website development, and employer outreach strategies
Quality assurance systems for job retention and client satisfaction
Collaboration with vocational training centers and community organizations
Personal Care
PERSONAL CARE SERVICES PROVIDER IN NEW JERSEY
SUPPORTING INDEPENDENCE AND DAILY LIVING THROUGH PERSONALIZED CARE
Personal Care Services in New Jersey provide essential assistance with daily living activities for individuals with disabilities, chronic illnesses, or age-related conditions. These services help maintain independence and enhance quality of life by offering support tailored to each individual’s needs. Personal Care Services are authorized under New Jersey Medicaid Home and Community-Based Services (HCBS) Waiver programs.
1. GOVERNING AGENCIES
Agency: New Jersey Department of Human Services (DHS)
Role: Administers Medicaid waiver funding for Personal Care Services and manages provider enrollment, service authorization, and reimbursement.
Agency: Division of Aging Services (DoAS)
Role: Ensures quality standards, service delivery, and compliance for Personal Care Services under HCBS waiver programs.
Agency: Centers for Medicare & Medicaid Services (CMS)
Role: Provides federal oversight ensuring Medicaid-funded Personal Care Services meet HCBS quality, person-centered planning, and participant protection standards.
2. PERSONAL CARE SERVICES OVERVIEW
Personal Care Services assist individuals with Activities of Daily Living (ADLs) and Instrumental Activities of Daily Living (IADLs) to maintain independence and well-being.
Approved providers may deliver:
Personal Hygiene Assistance: Bathing, grooming, oral care, and dressing.
Mobility Support: Transfers, ambulation, and positioning assistance.
Toileting and Incontinence Care: Support with bathroom use and hygiene maintenance.
Meal Preparation and Feeding: Preparing balanced meals, feeding assistance, and hydration support.
Housekeeping and Laundry: Light cleaning, bed making, and laundry tasks.
Medication Reminders: Non-skilled support with medication schedules.
Companionship and Social Engagement: Providing social interaction and light emotional support.
Safety Monitoring: Ensuring a safe environment and preventing accidents.
All services are delivered according to the Individualized Service Plan (ISP) to meet the participant’s specific care and safety needs.
3. LICENSING & PROVIDER APPROVAL REQUIREMENTS
Prerequisites:
Register the business entity with the New Jersey Division of Revenue and Enterprise Services.
Obtain EIN from the IRS and NPI (Type 2).
Enroll as a Medicaid Waiver Personal Care provider via the New Jersey Medicaid Provider Enrollment Portal.
Obtain licensure as a Personal Care Agency from DHS if applicable.
Maintain general liability and professional liability insurance.
Develop policies for personal care planning, safety protocols, and staff training.
Ensure staff meet background checks, health screenings, and training requirements.
4. NEW JERSEY PROVIDER ENROLLMENT PROCESS
Initial Interest and Application:
Complete the Provider Enrollment Application through the New Jersey Medicaid Provider Enrollment Portal for Personal Care Services under HCBS waivers.
Application and Documentation Submission:
Submit Articles of Incorporation, proof of EIN/NPI, insurance certificates, staff qualifications, and policy manuals.
Program Readiness Review:
DHS and DoAS evaluate provider readiness, including staff training, care protocols, and safety measures.
Approval & Medicaid Enrollment:
Upon approval, providers are authorized to bill Medicaid for Personal Care Services using designated billing codes.
5. REQUIRED DOCUMENTATION
Articles of Incorporation or Business License (New Jersey Division of Revenue)
IRS EIN confirmation
NPI confirmation
Personal Care Agency License (if applicable)
Proof of general and professional liability insurance
Personal Care Services Policy & Procedure Manual, including:
Participant intake, assessment, and individualized care planning procedures
Personal care assistance, hygiene, and mobility support guidelines
Staff credentialing, background checks, and training requirements
Documentation standards for care tracking and Medicaid billing
HIPAA compliance, participant rights, and grievance handling
Safety protocols, emergency response, and infection control measures
Quality assurance and compliance monitoring
6. STAFFING REQUIREMENTS
Role: Personal Care Program Director
Requirements: Bachelor’s degree in healthcare, social services, or a related field; supervisory experience preferred.
Role: Personal Care Aides (PCAs)
Requirements: High school diploma or GED; CPR/First Aid certification; training in personal care and ADL support; background clearance.
Role: Direct Support Professionals (DSPs)
Requirements: Experience in personal care and hygiene assistance; basic healthcare training; background clearance.
All staff must complete:
Personal care skills training, including ADLs and IADLs
Safety and infection control training
HIPAA compliance and participant rights education
Annual competency evaluations and professional development
Ongoing training in client safety and wellness monitoring
7. MEDICAID WAIVER PROGRAMS
Personal Care Services are available under the following New Jersey Medicaid Waivers:
Community Care Program for the Elderly and Disabled (CCPED)
Supports Program Waiver
Acquired Brain Injury (ABI) Waiver
Personal Care Assistant (PCA) Waiver
Home and Community-Based Services (HCBS) Waiver
Services may include:
Personal hygiene and grooming assistance
Mobility support and safety monitoring
Meal preparation and feeding assistance
Companionship and social support
Light housekeeping and personal environment maintenance
8. TIMELINE TO LAUNCH
Phase: Business Formation and Compliance Preparation
Timeline: 1–2 months
Phase: Staff Hiring, Credentialing, and Program Development
Timeline: 2–3 months
Phase: New Jersey Medicaid Provider Enrollment and Readiness Review
Timeline: 60–90 days
Phase: Medicaid Billing Setup and Personal Care Service Launch
Timeline: 30–45 days
9. CONTACT INFORMATION
New Jersey Department of Human Services (DHS)
Website: https://www.state.nj.us/humanservices/
Division of Aging Services (DoAS)
Website: https://www.state.nj.us/humanservices/doas/
New Jersey Medicaid Provider Enrollment Portal
Website: https://www.njmmis.com/
Centers for Medicare & Medicaid Services (CMS)
Website: https://www.cms.gov/
WAIVER CONSULTING GROUP’S START-UP ASSISTANCE SERVICE — NEW JERSEY PERSONAL CARE SERVICES PROVIDER
WCG supports agencies in launching Medicaid-compliant Personal Care Services in New Jersey, offering:
Scope of Work:
Business registration, Medicaid enrollment, and licensing assistance
Policy manual development for personal care planning and safety management
Staff credentialing, training program templates, and care documentation guidance
Medicaid billing setup and audit-prepared financial management
Branding, website development, and community outreach strategies
Quality assurance systems for personal care safety and compliance
Collaboration with healthcare providers and community organizations

Adaptive Equipment
ADAPTIVE EQUIPMENT SERVICES PROVIDER IN NEW JERSEY
ENHANCING MOBILITY AND INDEPENDENCE THROUGH CUSTOMIZED EQUIPMENT SOLUTIONS
Adaptive Equipment Services in New Jersey provide individuals with disabilities, chronic conditions, or mobility challenges with essential tools and devices to enhance their independence and quality of life. These services include assessment, procurement, customization, and maintenance of adaptive equipment. Adaptive Equipment Services are authorized under New Jersey Medicaid Home and Community-Based Services (HCBS) Waiver programs.
1. GOVERNING AGENCIES
Agency: New Jersey Department of Human Services (DHS)
Role: Administers Medicaid waiver funding for Adaptive Equipment Services and manages provider enrollment, service authorization, and reimbursement.
Agency: Division of Developmental Disabilities (DDD)
Role: Ensures quality standards, service delivery, and compliance for Adaptive Equipment Services under HCBS waiver programs.
Agency: Centers for Medicare & Medicaid Services (CMS)
Role: Provides federal oversight ensuring Medicaid-funded Adaptive Equipment Services meet HCBS quality, person-centered planning, and participant protection standards.
2. ADAPTIVE EQUIPMENT SERVICES OVERVIEW
Adaptive Equipment Services help individuals with disabilities to function more independently by providing customized tools and devices suited to their specific needs.
Approved providers may deliver:
Equipment Assessment: Evaluating the individual's needs and functional requirements.
Equipment Procurement: Sourcing mobility aids, communication devices, and other adaptive tools.
Customization and Fitting: Modifying equipment to meet the user’s physical and functional needs.
Installation and Setup: Ensuring the equipment is safely and correctly installed.
Training and Education: Teaching users and caregivers how to properly use and maintain the equipment.
Maintenance and Repair: Providing ongoing support to ensure the equipment remains functional and safe.
Technology Integration: Incorporating smart features or automation where applicable.
All services are delivered according to the Individualized Service Plan (ISP) to meet the participant’s adaptive and functional needs.
3. LICENSING & PROVIDER APPROVAL REQUIREMENTS
Prerequisites:
Register the business entity with the New Jersey Division of Revenue and Enterprise Services.
Obtain EIN from the IRS and NPI (Type 2).
Enroll as a Medicaid Waiver Adaptive Equipment provider via the New Jersey Medicaid Provider Enrollment Portal.
Obtain necessary certifications for equipment assessment, installation, and maintenance (if applicable).
Maintain general liability and professional liability insurance.
Develop policies for equipment assessment, installation, safety management, and maintenance.
Ensure staff meet background checks, health screenings, and technical training requirements.
4. NEW JERSEY PROVIDER ENROLLMENT PROCESS
Initial Interest and Application:
Complete the Provider Enrollment Application through the New Jersey Medicaid Provider Enrollment Portal for Adaptive Equipment Services under HCBS waivers.
Application and Documentation Submission:
Submit Articles of Incorporation, proof of EIN/NPI, insurance certificates, professional certifications, and policy manuals.
Program Readiness Review:
DHS and DDD evaluate provider readiness, including safety protocols, installation procedures, and staff qualifications.
Approval & Medicaid Enrollment:
Upon approval, providers are authorized to bill Medicaid for Adaptive Equipment Services using designated billing codes.
5. REQUIRED DOCUMENTATION
Articles of Incorporation or Business License (New Jersey Division of Revenue)
IRS EIN confirmation
NPI confirmation
Certifications for equipment installation and maintenance (if applicable)
Proof of general and professional liability insurance
Adaptive Equipment Services Policy & Procedure Manual including:
Needs assessment, equipment selection, and customization protocols
Installation, safety checks, and user training guidelines
Staff credentialing, background checks, and training records
Documentation standards for equipment tracking and Medicaid billing
HIPAA compliance, participant rights, and grievance handling
Safety protocols for device handling and maintenance
Quality assurance and compliance monitoring
6. STAFFING REQUIREMENTS
Role: Adaptive Equipment Program Director
Requirements: Bachelor’s degree in rehabilitation technology, healthcare administration, or related field; experience in adaptive equipment management.
Role: Assistive Technology Specialists
Requirements: Certification in adaptive equipment assessment and customization (e.g., Assistive Technology Professional (ATP)); experience with mobility aids and adaptive devices; background clearance.
Role: Support Technicians
Requirements: Technical training in equipment setup, repair, and maintenance; experience in customer support; background clearance.
All staff must complete:
Training in adaptive equipment installation and client safety
HIPAA compliance and client rights education
Ongoing professional development and certification updates
Annual competency evaluations and safety protocol refreshers
Maintenance and troubleshooting training
7. MEDICAID WAIVER PROGRAMS
Adaptive Equipment Services are available under the following New Jersey Medicaid Waivers:
Community Care Program for the Elderly and Disabled (CCPED)
Supports Program Waiver
Acquired Brain Injury (ABI) Waiver
Personal Care Assistant (PCA) Waiver
Home and Community-Based Services (HCBS) Waiver
Services may include:
Installation of mobility aids (e.g., wheelchairs, walkers, transfer devices)
Adaptive communication devices for speech, hearing, or vision impairments
Custom modifications for increased accessibility
Smart home adaptations for safety and control
Ongoing maintenance and repair of adaptive equipment
8. TIMELINE TO LAUNCH
Phase: Business Formation and Compliance Preparation
Timeline: 1–2 months
Phase: Staff Hiring, Credentialing, and Program Development
Timeline: 2–3 months
Phase: New Jersey Medicaid Provider Enrollment and Readiness Review
Timeline: 60–90 days
Phase: Medicaid Billing Setup and Adaptive Equipment Service Launch
Timeline: 30–45 days
9. CONTACT INFORMATION
New Jersey Department of Human Services (DHS)
Website: https://www.state.nj.us/humanservices/
Division of Developmental Disabilities (DDD)
Website: https://www.state.nj.us/humanservices/ddd/
New Jersey Medicaid Provider Enrollment Portal
Website: https://www.njmmis.com/
Centers for Medicare & Medicaid Services (CMS)
Website: https://www.cms.gov/
WAIVER CONSULTING GROUP’S START-UP ASSISTANCE SERVICE — NEW JERSEY ADAPTIVE EQUIPMENT SERVICES PROVIDER
WCG supports agencies in launching Medicaid-compliant Adaptive Equipment Services in New Jersey, offering:
Scope of Work:
Business registration, Medicaid enrollment, and licensing support
Policy manual development for adaptive equipment assessment and safety management
Staff credentialing, training program templates, and technical guidance
Medicaid billing setup and audit-prepared financial management
Branding, website development, and client engagement strategies
Quality assurance systems for equipment safety and maintenance compliance
Collaboration with healthcare providers and community organizations for referrals

Skilled Nursing
SKILLED NURSING SERVICES PROVIDER IN NEW JERSEY
DELIVERING MEDICAL CARE AND SUPPORT IN THE HOME AND COMMUNITY
Skilled Nursing Services in New Jersey provide medical care and support to individuals with chronic conditions, disabilities, or age-related health needs. These services are delivered by licensed nurses and include health monitoring, medication administration, wound care, and more. Skilled Nursing Services are authorized under New Jersey Medicaid Home and Community-Based Services (HCBS) Waiver programs.
1. GOVERNING AGENCIES
Agency: New Jersey Department of Human Services (DHS)
Role: Administers Medicaid waiver funding for Skilled Nursing Services and manages provider enrollment, service authorization, and reimbursement.
Agency: Division of Medical Assistance and Health Services (DMAHS)
Role: Oversees quality standards, service delivery, and compliance for Skilled Nursing Services under HCBS waiver programs.
Agency: Centers for Medicare & Medicaid Services (CMS)
Role: Provides federal oversight ensuring Medicaid-funded Skilled Nursing Services meet HCBS quality, person-centered planning, and participant protection standards.
2. SKILLED NURSING SERVICES OVERVIEW
Skilled Nursing Services are designed to provide medical care and health monitoring for individuals who require clinical support in their home or community settings.
Approved providers may deliver:
Health Assessments: Monitoring vital signs, assessing physical and mental health.
Medication Management: Administering medications and managing complex medication schedules.
Wound Care: Dressing changes, infection monitoring, and wound management.
Chronic Disease Management: Diabetes care, blood pressure monitoring, and respiratory therapy.
Tube Feeding and IV Therapy: Administering nutrition and medications through feeding tubes and intravenous methods.
Catheter and Ostomy Care: Maintenance, monitoring, and hygiene support.
Post-Surgical Care: Monitoring recovery and managing post-operative symptoms.
Health Education: Teaching patients and families to manage conditions effectively.
Emergency Care Plans: Developing and implementing care protocols for medical emergencies.
All services are delivered according to the Individualized Service Plan (ISP) to meet the participant’s medical and support needs.
3. LICENSING & PROVIDER APPROVAL REQUIREMENTS
Prerequisites:
Register the business entity with the New Jersey Division of Revenue and Enterprise Services.
Obtain EIN from the IRS and NPI (Type 2).
Enroll as a Medicaid Waiver Skilled Nursing provider via the New Jersey Medicaid Provider Enrollment Portal.
Obtain licensure as a Home Health Agency from the New Jersey Department of Health (NJDOH).
Maintain general liability and professional liability insurance.
Develop policies for clinical care, medication management, and safety protocols.
Ensure staff meet background checks, health screenings, and professional licensure requirements.
4. NEW JERSEY PROVIDER ENROLLMENT PROCESS
Initial Interest and Application:
Complete the Provider Enrollment Application through the New Jersey Medicaid Provider Enrollment Portal for Skilled Nursing Services under HCBS waivers.
Application and Documentation Submission:
Submit Articles of Incorporation, proof of EIN/NPI, nursing licenses, insurance certificates, and policy manuals.
Program Readiness Review:
DHS and DMAHS evaluate provider readiness, including clinical protocols, safety measures, and staff qualifications.
Approval & Medicaid Enrollment:
Upon approval, providers are authorized to bill Medicaid for Skilled Nursing Services using designated billing codes.
5. REQUIRED DOCUMENTATION
Articles of Incorporation or Business License (New Jersey Division of Revenue)
IRS EIN confirmation
NPI confirmation
Home Health Agency License (if applicable)
Proof of general and professional liability insurance
Skilled Nursing Services Policy & Procedure Manual including:
Health assessment, care planning, and medication management protocols
Staff credentialing, background checks, and ongoing training records
Documentation standards for clinical care tracking and Medicaid billing
HIPAA compliance, patient rights, and grievance handling
Infection control, safety protocols, and emergency response procedures
Quality assurance and compliance monitoring
6. STAFFING REQUIREMENTS
Role: Skilled Nursing Program Director
Requirements: Bachelor’s or Master’s degree in nursing; RN license in New Jersey; supervisory experience in clinical care.
Role: Registered Nurses (RNs)
Requirements: Valid RN license in New Jersey; experience in home healthcare; CPR/First Aid certification; background clearance.
Role: Licensed Practical Nurses (LPNs)
Requirements: Valid LPN license in New Jersey; experience in skilled nursing; CPR/First Aid certification; background clearance.
Role: Nursing Assistants (if applicable)
Requirements: CNA certification; supervised by an RN; background clearance.
All staff must complete:
Training in clinical protocols, medication management, and infection control
HIPAA compliance and patient rights education
Ongoing professional development and licensure renewal
Annual competency evaluations and safety protocol updates
CPR/First Aid and emergency response training
7. MEDICAID WAIVER PROGRAMS
Skilled Nursing Services are available under the following New Jersey Medicaid Waivers:
Community Care Program for the Elderly and Disabled (CCPED)
Supports Program Waiver
Acquired Brain Injury (ABI) Waiver
Personal Care Assistant (PCA) Waiver
Home and Community-Based Services (HCBS) Waiver
Services may include:
Health monitoring and chronic disease management
Medication administration and adherence support
Wound care and post-surgical monitoring
Tube feeding and catheter management
Emergency medical interventions and crisis care
8. TIMELINE TO LAUNCH
Phase: Business Formation and Compliance Preparation
Timeline: 1–2 months
Phase: Staff Hiring, Credentialing, and Program Development
Timeline: 2–3 months
Phase: New Jersey Medicaid Provider Enrollment and Readiness Review
Timeline: 60–90 days
Phase: Medicaid Billing Setup and Skilled Nursing Service Launch
Timeline: 30–45 days
9. CONTACT INFORMATION
New Jersey Department of Human Services (DHS)
Website: https://www.state.nj.us/humanservices/
Division of Medical Assistance and Health Services (DMAHS)
Website: https://www.state.nj.us/humanservices/dmahs/
New Jersey Department of Health (NJDOH)
Website: https://www.nj.gov/health/
New Jersey Medicaid Provider Enrollment Portal
Website: https://www.njmmis.com/
Centers for Medicare & Medicaid Services (CMS)
Website: https://www.cms.gov/
WAIVER CONSULTING GROUP’S START-UP ASSISTANCE SERVICE — NEW JERSEY SKILLED NURSING SERVICES PROVIDER
WCG supports agencies in launching Medicaid-compliant Skilled Nursing Services in New Jersey, offering:
Scope of Work:
Business registration, Medicaid enrollment, and licensing assistance
Policy manual development for clinical care and patient safety
Staff credentialing, training program templates, and compliance documentation
Medicaid billing setup and audit-prepared financial management
Branding, website development, and community outreach strategies
Quality assurance systems for clinical care and compliance monitoring
Collaboration with healthcare providers and community organizations

Adult Day Care
ADULT DAY CARE SERVICES PROVIDER IN NEW JERSEY
SUPPORTING WELL-BEING AND SOCIAL ENGAGEMENT THROUGH STRUCTURED DAY PROGRAMS
Adul Day Care Services in New Jersey provide structured, supervised care during daytime hours for individuals with disabilities, chronic conditions, or age-related challenges. These services focus on promoting social engagement, personal development, and maintaining functional abilities in a safe, supportive environment. Day Care Services are authorized under New Jersey Medicaid Home and Community-Based Services (HCBS) Waiver programs.
1. GOVERNING AGENCIES
Agency: New Jersey Department of Human Services (DHS)
Role: Administers Medicaid waiver funding for Adult Day Care Services and manages provider enrollment, service authorization, and reimbursement.
Agency: Division of Aging Services (DoAS)
Role: Oversees quality standards, service delivery, and compliance for Adult Day Care Services under HCBS waiver programs.
Agency: Centers for Medicare & Medicaid Services (CMS)
Role: Provides federal oversight ensuring Medicaid-funded Adult Day Care Services meet HCBS quality, person-centered planning, and participant protection standards.
2. ADULT DAY CARE SERVICES OVERVIEW
Day Care Services provide supervised activities, personal care, and social engagement to enhance quality of life and relieve family caregivers.
Approved providers may deliver:
Social and Recreational Activities: Group games, arts and crafts, music, and social events.
Personal Care Assistance: Help with Activities of Daily Living (ADLs) such as toileting, grooming, and mobility.
Health Monitoring: Basic wellness checks, medication reminders, and support for chronic conditions.
Cognitive Stimulation: Activities that promote memory, attention, and cognitive skills.
Nutritional Support: Meal and snack preparation tailored to dietary needs.
Exercise and Mobility Programs: Light physical activities to maintain strength and balance.
Caregiver Respite: Providing temporary relief for primary caregivers while ensuring participant safety.
Transportation: Rides to and from the day care center as needed.
All services are delivered according to the Individualized Service Plan (ISP) to meet the participant’s specific care needs and preferences.
3. LICENSING & PROVIDER APPROVAL REQUIREMENTS
Prerequisites:
Register the business entity with the New Jersey Division of Revenue and Enterprise Services.
Obtain EIN from the IRS and NPI (Type 2).
Enroll as a Medicaid Waiver Day Care provider via the New Jersey Medicaid Provider Enrollment Portal.
Obtain a Day Care License from the New Jersey Department of Health (NJDOH) if applicable.
Maintain general liability and professional liability insurance.
Develop policies for health monitoring, participant safety, and daily activity planning.
Ensure staff meet background checks, health screenings, and training requirements.
4. NEW JERSEY PROVIDER ENROLLMENT PROCESS
Initial Interest and Application:
Complete the Provider Enrollment Application through the New Jersey Medicaid Provider Enrollment Portal for Day Care Services under HCBS waivers.
Application and Documentation Submission:
Submit Articles of Incorporation, proof of EIN/NPI, insurance certificates, day care license, and policy manuals.
Program Readiness Review:
DHS and DoAS evaluate provider readiness, including activity planning, safety measures, and staff qualifications.
Approval & Medicaid Enrollment:
Upon approval, providers are authorized to bill Medicaid for Day Care Services using designated billing codes.
5. REQUIRED DOCUMENTATION
Articles of Incorporation or Business License (New Jersey Division of Revenue)
IRS EIN confirmation
NPI confirmation
Day Care License (if applicable)
Proof of general and professional liability insurance
Day Care Services Policy & Procedure Manual including:
Participant intake, assessment, and individualized care planning procedures
Daily activity programming and social engagement protocols
Staff credentialing, background checks, and ongoing training records
Documentation standards for care tracking and Medicaid billing
HIPAA compliance, participant rights, and grievance handling
Safety protocols, emergency response, and infection control measures
Quality assurance and compliance monitoring
6. STAFFING REQUIREMENTS
Role: Adult Day Care Program Director
Requirements: Bachelor’s degree in human services, healthcare administration, or related field; experience managing day programs.
Role: Direct Support Professionals (DSPs)
Requirements: High school diploma or GED; CPR/First Aid certification; experience in personal care and group activities; background clearance.
Role: Activity Coordinators
Requirements: Experience in planning and leading group activities; background clearance.
All staff must complete:
Training in activity planning and group management
HIPAA compliance and client rights education
Annual competency evaluations and ongoing professional development
Training in personal care assistance and wellness monitoring
Safety training, including emergency preparedness and infection control
7. MEDICAID WAIVER PROGRAMS
Adult day Care Services are available under the following New Jersey Medicaid Waivers:
Community Care Program for the Elderly and Disabled (CCPED)
Supports Program Waiver
Acquired Brain Injury (ABI) Waiver
Personal Care Assistant (PCA) Waiver
Home and Community-Based Services (HCBS) Waiver
Services may include:
Social engagement and cognitive stimulation
Personal care and hygiene assistance
Recreational and therapeutic activities
Health monitoring and wellness support
Nutritional meals and dietary management
Transportation to and from the day care center
8. TIMELINE TO LAUNCH
Phase: Business Formation and Compliance Preparation
Timeline: 1–2 months
Phase: Staff Hiring, Credentialing, and Program Development
Timeline: 2–3 months
Phase: New Jersey Medicaid Provider Enrollment and Readiness Review
Timeline: 60–90 days
Phase: Medicaid Billing Setup and Day Care Service Launch
Timeline: 30–45 days
9. CONTACT INFORMATION
New Jersey Department of Human Services (DHS)
Website: https://www.state.nj.us/humanservices/
Division of Aging Services (DoAS)
Website: https://www.state.nj.us/humanservices/doas/
New Jersey Medicaid Provider Enrollment Portal
Website: https://www.njmmis.com/
Centers for Medicare & Medicaid Services (CMS)
Website: https://www.cms.gov/
WAIVER CONSULTING GROUP’S START-UP ASSISTANCE SERVICE — NEW JERSEY ADULT DAY CARE SERVICES PROVIDER
WCG supports agencies in launching Medicaid-compliant Day Care Services in New Jersey, offering:
Scope of Work:
Business registration, Medicaid enrollment, and licensing assistance
Policy manual development for day program planning and participant safety
Staff credentialing, training program templates, and activity documentation guidance
Medicaid billing setup and audit-prepared financial management
Branding, website development, and client engagement strategies
Quality assurance systems for activity safety and compliance
Collaboration with healthcare providers and community organizations

Assistive Technology
ASSISTIVE TECHNOLOGY SERVICES PROVIDER IN NEW JERSEY
ENHANCING INDEPENDENCE THROUGH TECHNOLOGICAL INNOVATION AND SUPPORT
Assistive Technology Services in New Jersey provide adaptive tools and equipment to help individuals with disabilities or mobility challenges live independently. These services focus on evaluating needs, selecting devices, and providing training to maximize functionality and quality of life. Assistive Technology Services are authorized under New Jersey Medicaid Home and Community-Based Services (HCBS) Waiver programs.
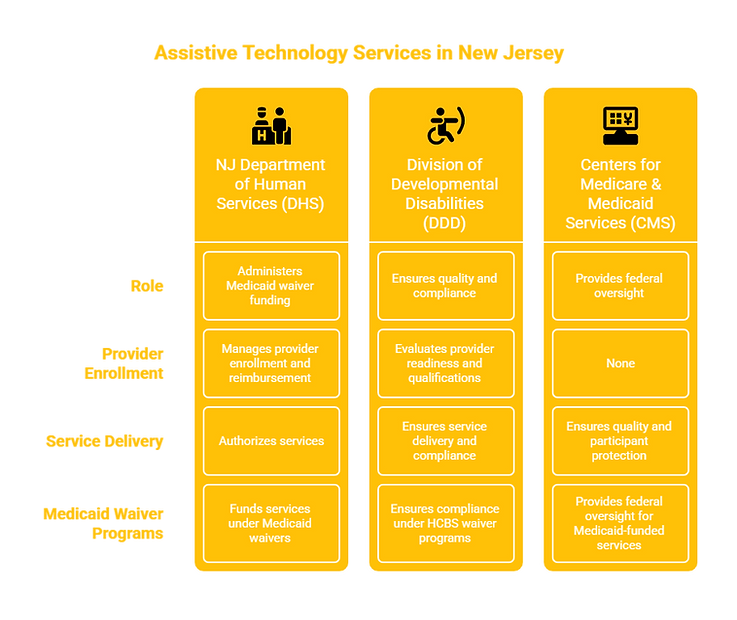
1. GOVERNING AGENCIES
Agency: New Jersey Department of Human Services (DHS)
Role: Administers Medicaid waiver funding for Assistive Technology Services and manages provider enrollment, service authorization, and reimbursement.
Agency: Division of Developmental Disabilities (DDD)
Role: Ensures quality standards, service delivery, and compliance for Assistive Technology Services under HCBS waiver programs.
Agency: Centers for Medicare & Medicaid Services (CMS)
Role: Provides federal oversight ensuring Medicaid-funded Assistive Technology Services meet HCBS quality, person-centered planning, and participant protection standards.
2. ASSISTIVE TECHNOLOGY SERVICES OVERVIEW
Assistive Technology Services enhance daily living by offering devices and tools that support physical, sensory, or cognitive impairments.
Approved providers may deliver:
Needs Assessment: Evaluating individual requirements for adaptive devices.
Device Selection: Recommending tools such as mobility aids, communication devices, or adaptive household equipment.
Installation and Setup: Setting up devices in the home or community setting.
User Training: Educating individuals and caregivers on the proper use and maintenance of assistive technology.
Device Maintenance: Providing ongoing support, repair, and technical assistance.
Adaptive Communication Devices: Speech-generating devices, hearing aids, and visual aids.
Environmental Controls: Home automation solutions for accessibility and safety.
All services are provided according to the Individualized Service Plan (ISP) to meet the participant’s specific needs.
3. LICENSING & PROVIDER APPROVAL REQUIREMENTS
Prerequisites:
Register the business entity with the New Jersey Division of Revenue and Enterprise Services.
Obtain EIN from the IRS and NPI (Type 2).
Enroll as a Medicaid Waiver Assistive Technology provider via the New Jersey Medicaid Provider Enrollment Portal.
Obtain any required certification for device installation and technical support.
Maintain general liability and professional liability insurance.
Develop policies for equipment assessment, installation, and safety management.
Ensure staff meet background checks, health screenings, and technical training requirements.
4. NEW JERSEY PROVIDER ENROLLMENT PROCESS
Initial Interest and Application:
Complete the Provider Enrollment Application through the New Jersey Medicaid Provider Enrollment Portal for Assistive Technology Services under HCBS waivers.
Application and Documentation Submission:
Submit Articles of Incorporation, proof of EIN/NPI, insurance certificates, professional certifications, and policy manuals.
Program Readiness Review:
DHS and DDD evaluate provider readiness, including safety protocols, installation procedures, and staff qualifications.
Approval & Medicaid Enrollment:
Upon approval, providers are authorized to bill Medicaid for Assistive Technology Services using designated billing codes.
5. REQUIRED DOCUMENTATION
Articles of Incorporation or Business License (New Jersey Division of Revenue)
IRS EIN confirmation
NPI confirmation
Professional certifications (e.g., Assistive Technology Professional (ATP))
Proof of general and professional liability insurance
Assistive Technology Services Policy & Procedure Manual including:
Needs assessment, device selection, and installation protocols
Maintenance, troubleshooting, and user training procedures
Staff credentialing, background checks, and ongoing training records
HIPAA compliance, client rights, and grievance handling
Documentation standards for device usage tracking and Medicaid billing
Safety protocols, emergency response, and maintenance schedules
Quality assurance and compliance monitoring
6. STAFFING REQUIREMENTS
Role: Assistive Technology Program Director
Requirements: Bachelor’s degree in rehabilitation technology, healthcare administration, or related field; certification as an Assistive Technology Professional (ATP) preferred.
Role: Assistive Technology Specialists
Requirements: Certification in assistive technology assessment and device implementation; experience with mobility aids and adaptive devices; background clearance.
Role: Support Technicians
Requirements: Technical training in device setup and repair; experience in customer support and maintenance services.
All staff must complete:
Training in adaptive equipment installation and client safety
HIPAA compliance and client rights education
Ongoing professional development and technical certification updates
Annual competency evaluations and safety protocol refreshers
7. MEDICAID WAIVER PROGRAMS
Assistive Technology Services are available under the following New Jersey Medicaid Waivers:
Community Care Program for the Elderly and Disabled (CCPED)
Supports Program Waiver
Acquired Brain Injury (ABI) Waiver
Personal Care Assistant (PCA) Waiver
Home and Community-Based Services (HCBS) Waiver
Services may include:
Installation of mobility aids (e.g., wheelchairs, walkers, transfer devices)
Adaptive communication devices for speech, hearing, or vision impairments
Smart home adaptations for safety and accessibility
Technology training for individuals and caregivers
Equipment maintenance and repair services
8. TIMELINE TO LAUNCH
Phase: Business Formation and Compliance Preparation
Timeline: 1–2 months
Phase: Staff Hiring, Credentialing, and Program Development
Timeline: 2–3 months
Phase: New Jersey Medicaid Provider Enrollment and Readiness Review
Timeline: 60–90 days
Phase: Medicaid Billing Setup and Assistive Technology Service Launch
Timeline: 30–45 days
9. CONTACT INFORMATION
New Jersey Department of Human Services (DHS)
Website: https://www.state.nj.us/humanservices/
Division of Developmental Disabilities (DDD)
Website: https://www.state.nj.us/humanservices/ddd/
New Jersey Medicaid Provider Enrollment Portal
Website: https://www.njmmis.com/
Centers for Medicare & Medicaid Services (CMS)
Website: https://www.cms.gov/
WAIVER CONSULTING GROUP’S START-UP ASSISTANCE SERVICE — NEW JERSEY ASSISTIVE TECHNOLOGY SERVICES PROVIDER
WCG supports healthcare agencies and adaptive technology providers in launching Medicaid-compliant Assistive Technology Services in New Jersey, offering:
Scope of Work:
Business registration, Medicaid enrollment, and licensing support
Policy manual development for adaptive equipment planning and safety management
Staff credentialing, training program templates, and technical guidance
Medicaid billing setup and audit-prepared financial management
Branding, website development, and client engagement strategies
Quality assurance systems for device safety, user satisfaction, and compliance
Collaboration with healthcare providers and community organizations for referrals
Behavioral Support
BEHAVIORAL SUPPORT SERVICES PROVIDER IN NEW JERSEY
PROMOTING POSITIVE BEHAVIORS AND WELL-BEING THROUGH STRUCTURED INTERVENTIONS
Behavioral Support Services in New Jersey provide therapeutic interventions to help individuals experiencing behavioral challenges or developmental disabilities. These services focus on enhancing coping strategies, reducing maladaptive behaviors, and promoting positive social interactions. Behavioral Support Services are authorized under New Jersey Medicaid Home and Community-Based Services (HCBS) Waiver programs.
1. GOVERNING AGENCIES
Agency: New Jersey Department of Human Services (DHS)
Role: Administers Medicaid waiver funding for Behavioral Support Services and manages provider enrollment, service authorization, and reimbursement.
Agency: Division of Developmental Disabilities (DDD)
Role: Ensures quality standards, service delivery, and compliance for Behavioral Support Services under HCBS waiver programs.
Agency: Centers for Medicare & Medicaid Services (CMS)
Role: Provides federal oversight ensuring Medicaid-funded Behavioral Support Services meet HCBS quality, person-centered planning, and participant protection standards.
2. BEHAVIORAL SUPPORT SERVICES OVERVIEW
Behavioral Support Services help individuals develop coping mechanisms and positive behaviors, fostering personal growth and community integration.
Approved providers may deliver:
Behavioral Assessment: Identifying triggers, patterns, and underlying causes of challenging behaviors.
Behavioral Intervention Planning: Developing individualized strategies to address maladaptive behaviors.
Positive Behavior Support (PBS): Implementing structured plans to encourage appropriate behaviors.
Crisis Intervention: De-escalating situations and implementing safety measures during behavioral crises.
Skill Building: Teaching coping skills, social interactions, and self-regulation techniques.
Family and Caregiver Training: Educating families on behavior management strategies.
Behavioral Monitoring: Tracking progress and adjusting intervention plans as needed.
Social Skills Development: Fostering communication, relationship building, and problem-solving abilities.
All services are delivered according to the Individualized Service Plan (ISP) to meet the participant’s behavioral health and support needs.
3. LICENSING & PROVIDER APPROVAL REQUIREMENTS
Prerequisites:
Register the business entity with the New Jersey Division of Revenue and Enterprise Services.
Obtain EIN from the IRS and NPI (Type 2).
Enroll as a Medicaid Waiver Behavioral Support provider via the New Jersey Medicaid Provider Enrollment Portal.
Obtain licensure from DHS as a behavioral health service provider if applicable.
Maintain general liability and professional liability insurance.
Develop comprehensive policies for behavioral intervention, crisis management, and caregiver support.
Ensure staff meet background checks, health screenings, and behavioral support training requirements.
4. NEW JERSEY PROVIDER ENROLLMENT PROCESS
Initial Interest and Application:
Complete the Provider Enrollment Application through the New Jersey Medicaid Provider Enrollment Portal for Behavioral Support Services under HCBS waivers.
Application and Documentation Submission:
Submit Articles of Incorporation, proof of EIN/NPI, insurance certificates, professional licenses, and policy manuals.
Program Readiness Review:
DHS and DDD evaluate provider readiness, including behavioral support protocols, safety measures, and staff qualifications.
Approval & Medicaid Enrollment:
Upon approval, providers are authorized to bill Medicaid for Behavioral Support Services using designated billing codes.
5. REQUIRED DOCUMENTATION
Articles of Incorporation or Business License (New Jersey Division of Revenue)
IRS EIN confirmation
NPI confirmation
Professional Licenses (e.g., Licensed Behavioral Analyst, Social Worker)
Proof of general and professional liability insurance
Behavioral Support Services Policy & Procedure Manual including:
Behavioral assessment, intervention planning, and crisis management protocols
Staff credentialing, background checks, and ongoing training records
Documentation standards for behavioral tracking and Medicaid billing
HIPAA compliance, client rights, and grievance handling
Safety protocols for therapeutic settings and participant interactions
Crisis de-escalation, safety planning, and emergency response measures
Quality assurance and compliance monitoring
6. STAFFING REQUIREMENTS
Role: Behavioral Support Program Director
Requirements: Master’s degree in psychology, social work, or applied behavior analysis; state licensure; experience in program management.
Role: Behavioral Support Specialists
Requirements: Licensed Behavioral Analysts (LBA), Licensed Clinical Social Workers (LCSW), or Licensed Mental Health Counselors (LMHC); background clearance.
Role: Behavioral Technicians
Requirements: Certification in behavioral analysis or related field; supervised by a licensed professional; experience in direct behavioral support.
Role: Family Support Coordinators
Requirements: Experience in training caregivers and providing behavioral guidance; background clearance.
All staff must complete:
Training in behavioral intervention techniques and positive behavior support
HIPAA compliance and client rights education
Annual competency evaluations and ongoing professional development
Crisis management and de-escalation techniques
Ongoing training in therapeutic approaches and behavior monitoring
7. MEDICAID WAIVER PROGRAMS
Behavioral Support Services are available under the following New Jersey Medicaid Waivers:
Community Care Program for the Elderly and Disabled (CCPED)
Supports Program Waiver
Acquired Brain Injury (ABI) Waiver
Personal Care Assistant (PCA) Waiver
Home and Community-Based Services (HCBS) Waiver
Services may include:
Individual and group therapy focusing on behavior management
Crisis intervention and behavioral de-escalation
Social skills training and communication enhancement
Caregiver education and family support sessions
Ongoing behavioral monitoring and adjustment of care plans
8. TIMELINE TO LAUNCH
Phase: Business Formation and Compliance Preparation
Timeline: 1–2 months
Phase: Staff Hiring, Credentialing, and Program Development
Timeline: 2–3 months
Phase: New Jersey Medicaid Provider Enrollment and Readiness Review
Timeline: 60–90 days
Phase: Medicaid Billing Setup and Behavioral Support Service Launch
Timeline: 30–45 days
9. CONTACT INFORMATION
New Jersey Department of Human Services (DHS)
Website: https://www.state.nj.us/humanservices/
Division of Developmental Disabilities (DDD)
Website: https://www.state.nj.us/humanservices/ddd/
New Jersey Medicaid Provider Enrollment Portal
Website: https://www.njmmis.com/
Centers for Medicare & Medicaid Services (CMS)
Website: https://www.cms.gov/
WAIVER CONSULTING GROUP’S START-UP ASSISTANCE SERVICE — NEW JERSEY BEHAVIORAL SUPPORT SERVICES PROVIDER
WCG supports agencies in launching Medicaid-compliant Behavioral Support Services in New Jersey, offering:
Scope of Work:
Business registration, Medicaid enrollment, and licensing assistance
Policy manual development for behavioral support and crisis management
Staff credentialing, training program templates, and compliance documentation
Medicaid billing setup and audit-prepared financial management
Branding, website development, and caregiver support strategies
Quality assurance systems for behavior tracking and therapeutic outcomes

Home Modification
HOME MODIFICATION SERVICES PROVIDER IN NEW JERSEY
IMPROVING ACCESSIBILITY AND SAFETY THROUGH CUSTOMIZED HOME ADAPTATIONS
Home Modification Services in New Jersey support individuals with disabilities, chronic conditions, or mobility challenges by providing adaptive modifications to their living environments. These services help ensure that homes are safe, accessible, and conducive to independent living. Home Modification Services are authorized under New Jersey Medicaid Home and Community-Based Services (HCBS) Waiver programs.
1. GOVERNING AGENCIES
Agency: New Jersey Department of Human Services (DHS)
Role: Administers Medicaid waiver funding for Home Modification Services and manages provider enrollment, service authorization, and reimbursement.
Agency: Division of Developmental Disabilities (DDD)
Role: Ensures quality standards, service delivery, and compliance for Home Modification Services under HCBS waiver programs.
Agency: Centers for Medicare & Medicaid Services (CMS)
Role: Provides federal oversight ensuring Medicaid-funded Home Modification Services meet HCBS quality, person-centered planning, and participant protection standards.
2. HOME MODIFICATION SERVICES OVERVIEW
Home Modification Services are designed to make living environments more accessible and safe for individuals with physical or cognitive disabilities.
Approved providers may deliver:
Accessibility Improvements: Installation of ramps, widened doorways, and handrails.
Bathroom Modifications: Roll-in showers, grab bars, accessible sinks, and raised toilet seats.
Kitchen Adjustments: Lowered countertops, accessible cabinets, and adapted appliances.
Safety Enhancements: Installation of safety alarms, improved lighting, and slip-resistant flooring.
Mobility Aids: Stairlifts, vertical platform lifts, and grab bars.
Home Automation Integration: Smart home technologies for lighting, temperature, and security management.
Structural Modifications: Door widening, hallway adjustments, and entryway improvements.
All modifications are delivered according to the Individualized Service Plan (ISP) and based on a professional assessment of the participant’s needs.
3. LICENSING & PROVIDER APPROVAL REQUIREMENTS
Prerequisites:
Register the business entity with the New Jersey Division of Revenue and Enterprise Services.
Obtain EIN from the IRS and NPI (Type 2).
Enroll as a Medicaid Waiver Home Modification provider via the New Jersey Medicaid Provider Enrollment Portal.
Obtain any required contractor licenses from the New Jersey Division of Consumer Affairs.
Maintain general liability and professional liability insurance.
Develop comprehensive policies for safety, project planning, and quality assurance.
Ensure contractors and subcontractors meet background checks and licensing requirements.
4. NEW JERSEY PROVIDER ENROLLMENT PROCESS
Initial Interest and Application:
Complete the Provider Enrollment Application through the New Jersey Medicaid Provider Enrollment Portal for Home Modification Services under HCBS waivers.
Application and Documentation Submission:
Submit Articles of Incorporation, proof of EIN/NPI, contractor licenses, insurance certificates, and policy manuals.
Program Readiness Review:
DHS and DDD evaluate provider readiness, including safety procedures, modification protocols, and contractor qualifications.
Approval & Medicaid Enrollment:
Upon approval, providers are authorized to bill Medicaid for Home Modification Services using designated billing codes.
5. REQUIRED DOCUMENTATION
Articles of Incorporation or Business License (New Jersey Division of Revenue)
IRS EIN confirmation
NPI confirmation
Contractor Licenses (if applicable)
Proof of general and professional liability insurance
Home Modification Services Policy & Procedure Manual including:
Safety and risk assessment protocols
Project planning and modification guidelines
Contractor vetting, background checks, and credential verification
Compliance with building codes, ADA standards, and safety regulations
Documentation standards for project tracking and Medicaid billing
Risk management and emergency preparedness procedures
Quality assurance and compliance monitoring
6. STAFFING REQUIREMENTS
Role: Home Modification Program Director
Requirements: Bachelor’s degree in construction management, healthcare administration, or related field; experience managing home accessibility projects.
Role: Licensed Contractors
Requirements: State contractor license; experience in home modifications for accessibility; background clearance.
Role: Accessibility Specialists
Requirements: Certification in home accessibility modifications (e.g., CAPS - Certified Aging-in-Place Specialist); background clearance.
All staff must complete:
Safety training and risk management education
HIPAA compliance and client rights training
Ongoing professional development and continuing education
Annual competency evaluations and safety protocol updates
7. MEDICAID WAIVER PROGRAMS
Home Modification Services are available under the following New Jersey Medicaid Waivers:
Community Care Program for the Elderly and Disabled (CCPED)
Supports Program Waiver
Acquired Brain Injury (ABI) Waiver
Personal Care Assistant (PCA) Waiver
Home and Community-Based Services (HCBS) Waiver
Services may include:
Installation of wheelchair ramps and accessible doorways
Bathroom accessibility improvements (e.g., roll-in showers, grab bars)
Kitchen modifications to accommodate mobility aids
Safety enhancements and adaptive equipment installations
Smart home integration for individuals with mobility impairments
8. TIMELINE TO LAUNCH
Phase: Business Formation and Compliance Preparation
Timeline: 1–2 months
Phase: Staff Hiring, Credentialing, and Program Development
Timeline: 2–3 months
Phase: New Jersey Medicaid Provider Enrollment and Readiness Review
Timeline: 60–90 days
Phase: Medicaid Billing Setup and Home Modification Service Launch
Timeline: 30–45 days
9. CONTACT INFORMATION
New Jersey Department of Human Services (DHS)
Website: https://www.state.nj.us/humanservices/
Division of Developmental Disabilities (DDD)
Website: https://www.state.nj.us/humanservices/ddd/
New Jersey Division of Consumer Affairs
Website: https://www.njconsumeraffairs.gov/
New Jersey Medicaid Provider Enrollment Portal
Website: https://www.njmmis.com/
Centers for Medicare & Medicaid Services (CMS)
Website: https://www.cms.gov/
WAIVER CONSULTING GROUP’S START-UP ASSISTANCE SERVICE — NEW JERSEY HOME MODIFICATION SERVICES PROVIDER
WCG supports agencies in launching Medicaid-compliant Home Modification Services in New Jersey, offering:
Scope of Work:
Business registration, Medicaid enrollment, and licensing support
Policy manual development for accessibility planning and safety compliance
Staff credentialing, training program templates, and project documentation guidance
Medicaid billing setup and project management support
Branding, website development, and client engagement strategies
Quality assurance systems for safety monitoring and compliance
Collaboration with healthcare providers and community organizations for referrals

Cognitive Rehabilitation
COGNITIVE REHABILITATION SERVICES PROVIDER IN NEW JERSEY
ENHANCING COGNITIVE FUNCTION THROUGH TARGETED THERAPEUTIC INTERVENTIONS
Cognitive Rehabilitation Services in New Jersey provide therapeutic interventions to help individuals with cognitive impairments regain or improve their thinking skills, memory, attention, and problem-solving abilities. These services are essential for individuals recovering from brain injuries, strokes, or those living with neurological conditions. Cognitive Rehabilitation Services are authorized under New Jersey Medicaid Home and Community-Based Services (HCBS) Waiver programs.
1. GOVERNING AGENCIES
Agency: New Jersey Department of Human Services (DHS)
Role: Administers Medicaid waiver funding for Cognitive Rehabilitation Services and manages provider enrollment, service authorization, and reimbursement.
Agency: Division of Developmental Disabilities (DDD)
Role: Ensures quality standards, service delivery, and compliance for Cognitive Rehabilitation Services under HCBS waiver programs.
Agency: Centers for Medicare & Medicaid Services (CMS)
Role: Provides federal oversight ensuring Medicaid-funded Cognitive Rehabilitation Services meet HCBS quality, person-centered planning, and participant protection standards.
2. COGNITIVE REHABILITATION SERVICES OVERVIEW
Cognitive Rehabilitation Services are designed to support individuals with cognitive challenges by using structured activities and therapeutic exercises to enhance cognitive functioning.
Approved providers may deliver:
Cognitive Skills Training: Exercises to improve memory, attention, problem-solving, and reasoning.
Compensatory Strategy Training: Teaching techniques to manage cognitive deficits in daily life.
Executive Function Coaching: Enhancing planning, organization, and task management skills.
Memory Rehabilitation: Techniques to improve short-term and long-term memory retention.
Attention Training: Improving focus and concentration through structured activities.
Social Cognition Therapy: Developing communication and social interaction skills.
Community Reintegration: Assisting individuals in applying cognitive skills in real-world settings.
Support for Caregivers: Training and guidance to help families understand and manage cognitive challenges.
All services are delivered according to the Individualized Service Plan (ISP) to meet the participant’s cognitive and functional needs.
3. LICENSING & PROVIDER APPROVAL REQUIREMENTS
Prerequisites:
Register the business entity with the New Jersey Division of Revenue and Enterprise Services.
Obtain EIN from the IRS and NPI (Type 2).
Enroll as a Medicaid Waiver Cognitive Rehabilitation provider via the New Jersey Medicaid Provider Enrollment Portal.
Obtain licensure from DHS if applicable.
Maintain general liability and professional liability insurance.
Develop policies for therapeutic interventions, safety protocols, and caregiver support.
Ensure staff meet background checks, health screenings, and professional certification requirements.
4. NEW JERSEY PROVIDER ENROLLMENT PROCESS
Initial Interest and Application:
Complete the Provider Enrollment Application through the New Jersey Medicaid Provider Enrollment Portal for Cognitive Rehabilitation Services under HCBS waivers.
Application and Documentation Submission:
Submit Articles of Incorporation, proof of EIN/NPI, professional licenses, insurance certificates, and policy manuals.
Program Readiness Review:
DHS and DDD evaluate provider readiness, including therapy protocols, safety measures, and staff qualifications.
Approval & Medicaid Enrollment:
Upon approval, providers are authorized to bill Medicaid for Cognitive Rehabilitation Services using designated billing codes.
5. REQUIRED DOCUMENTATION
Articles of Incorporation or Business License (New Jersey Division of Revenue)
IRS EIN confirmation
NPI confirmation
Professional Licenses (e.g., Certified Brain Injury Specialist, Occupational Therapist)
Proof of general and professional liability insurance
Cognitive Rehabilitation Services Policy & Procedure Manual including:
Cognitive assessment, therapy planning, and intervention protocols
Staff credentialing, background checks, and ongoing training records
Documentation standards for progress tracking and Medicaid billing
HIPAA compliance, client rights, and grievance handling
Safety protocols for therapeutic settings and patient interactions
Emergency response, crisis management, and safety measures
Quality assurance and compliance monitoring
6. STAFFING REQUIREMENTS
Role: Cognitive Rehabilitation Program Director
Requirements: Master’s degree in psychology, occupational therapy, or related field; certification in brain injury rehabilitation; experience in program management.
Role: Cognitive Rehabilitation Therapists
Requirements: Licensed Occupational Therapists (OTs), Speech-Language Pathologists (SLPs), or Certified Brain Injury Specialists (CBIS); experience in cognitive rehabilitation; background clearance.
Role: Cognitive Rehabilitation Assistants
Requirements: Bachelor’s degree in psychology, neuroscience, or related field; supervised by a licensed therapist; background clearance.
All staff must complete:
Training in cognitive therapy techniques and rehabilitation planning
HIPAA compliance and client rights education
Annual competency evaluations and ongoing professional development
Safety and emergency preparedness training
Ongoing training in brain injury management and cognitive support
7. MEDICAID WAIVER PROGRAMS
Cognitive Rehabilitation Services are available under the following New Jersey Medicaid Waivers:
Community Care Program for the Elderly and Disabled (CCPED)
Supports Program Waiver
Acquired Brain Injury (ABI) Waiver
Personal Care Assistant (PCA) Waiver
Home and Community-Based Services (HCBS) Waiver
Services may include:
Cognitive skill training and memory enhancement
Problem-solving and executive function support
Attention and focus improvement exercises
Social cognition and communication skills training
Community reintegration and practical skill application
8. TIMELINE TO LAUNCH
Phase: Business Formation and Compliance Preparation
Timeline: 1–2 months
Phase: Staff Hiring, Credentialing, and Program Development
Timeline: 2–3 months
Phase: New Jersey Medicaid Provider Enrollment and Readiness Review
Timeline: 60–90 days
Phase: Medicaid Billing Setup and Cognitive Rehabilitation Service Launch
Timeline: 30–45 days
9. CONTACT INFORMATION
New Jersey Department of Human Services (DHS)
Website: https://www.state.nj.us/humanservices/
Division of Developmental Disabilities (DDD)
Website: https://www.state.nj.us/humanservices/ddd/
New Jersey Medicaid Provider Enrollment Portal
Website: https://www.njmmis.com/
Centers for Medicare & Medicaid Services (CMS)
Website: https://www.cms.gov/
WAIVER CONSULTING GROUP’S START-UP ASSISTANCE SERVICE — NEW JERSEY COGNITIVE REHABILITATION SERVICES PROVIDER
WCG supports agencies in launching Medicaid-compliant Cognitive Rehabilitation Services in New Jersey, offering:
Scope of Work:
Business registration, Medicaid enrollment, and licensing assistance
Policy manual development for cognitive therapy planning and safety management
Staff credentialing, training program templates, and cognitive rehabilitation documentation guidance
Medicaid billing setup and audit-prepared financial management
Branding, website development, and community outreach strategies
Quality assurance systems for therapeutic efficacy and compliance
Collaboration with healthcare providers for integrated care planning

In-Home & Community Services
IN-HOME AND COMMUNITY-BASED SERVICES PROVIDER IN NEW JERSEY
PROMOTING INDEPENDENCE AND WELL-BEING THROUGH PERSON-CENTERED SUPPORT IN THE COMMUNITY
In-Home and Community-Based Services (HCBS) in New Jersey provide essential support to individuals with disabilities, chronic conditions, or age-related challenges. These services are designed to promote independence and enhance quality of life by offering assistance in the home or community setting. HCBS are authorized under New Jersey Medicaid Home and Community-Based Services Waiver programs.
1. GOVERNING AGENCIES
Agency: New Jersey Department of Human Services (DHS)
Role: Administers Medicaid waiver funding for In-Home and Community-Based Services and manages provider enrollment, service authorization, and reimbursement.
Agency: Division of Aging Services (DoAS)
Role: Ensures quality standards, service delivery, and compliance for HCBS under Medicaid waiver programs.
Agency: Division of Developmental Disabilities (DDD)
Role: Oversees service coordination, eligibility, and quality for individuals with developmental disabilities.
Agency: Centers for Medicare & Medicaid Services (CMS)
Role: Provides federal oversight ensuring Medicaid-funded HCBS meet quality standards, person-centered planning, and participant protection requirements.
2. IN-HOME AND COMMUNITY-BASED SERVICES OVERVIEW
HCBS provide support services tailored to the needs of individuals in their own homes or community settings, helping them maintain independence and participate in their communities.
Approved providers may deliver:
Personal Care Assistance: Support with Activities of Daily Living (ADLs) like bathing, grooming, feeding, and mobility.
Homemaker Services: Light housekeeping, meal preparation, laundry, and grocery shopping.
Respite Care: Temporary relief for family caregivers.
Skilled Nursing: Health monitoring, medication administration, and basic medical care.
Behavioral Support: Addressing behavioral challenges and promoting positive social interactions.
Case Management: Coordinating care and connecting individuals with community resources.
Transportation Services: Safe and reliable transport to medical appointments, community activities, and social engagements.
Day Habilitation: Structured activities to build social, cognitive, and physical skills.
Supported Employment: Assistance with finding and maintaining community-based jobs.
Home Modifications: Installing ramps, handrails, and accessibility features.
All services are delivered according to the Individualized Service Plan (ISP) to meet the participant’s needs and preferences.
3. LICENSING & PROVIDER APPROVAL REQUIREMENTS
Prerequisites:
Register the business entity with the New Jersey Division of Revenue and Enterprise Services.
Obtain EIN from the IRS and NPI (Type 2).
Enroll as a Medicaid Waiver HCBS provider via the New Jersey Medicaid Provider Enrollment Portal.
Obtain required licenses or certifications for specific services (e.g., nursing, behavioral support).
Maintain general liability and professional liability insurance.
Develop policies for service planning, health monitoring, and client safety.
Ensure staff meet background checks, health screenings, and training requirements.
4. NEW JERSEY PROVIDER ENROLLMENT PROCESS
Initial Interest and Application:
Complete the Provider Enrollment Application through the New Jersey Medicaid Provider Enrollment Portal for HCBS.
Application and Documentation Submission:
Submit Articles of Incorporation, proof of EIN/NPI, insurance certificates, staff qualifications, and service-specific licenses.
Program Readiness Review:
DHS and DoAS/DDD evaluate provider readiness, including safety protocols, care plans, and staff qualifications.
Approval & Medicaid Enrollment:
Upon approval, providers are authorized to bill Medicaid for HCBS using designated billing codes.
5. REQUIRED DOCUMENTATION
Articles of Incorporation or Business License (New Jersey Division of Revenue)
IRS EIN confirmation
NPI confirmation
Licenses for specialized services (e.g., nursing, behavioral support)
Proof of general and professional liability insurance
HCBS Policy & Procedure Manual including:
Participant intake, assessment, and service planning protocols
Personal care assistance, homemaker tasks, and respite care guidelines
Staff credentialing, background checks, and training requirements
Documentation standards for service tracking and Medicaid billing
HIPAA compliance, participant rights, and grievance handling
Safety protocols, emergency response, and infection control measures
Quality assurance and compliance monitoring
6. STAFFING REQUIREMENTS
Role: HCBS Program Director
Requirements: Bachelor’s degree in healthcare, human services, or related field; supervisory experience preferred.
Role: Direct Support Professionals (DSPs)
Requirements: High school diploma or GED; CPR/First Aid certification; training in ADLs and IADLs support; background clearance.
Role: Nurses (if applicable)
Requirements: Valid RN or LPN license in New Jersey; experience in home healthcare; background clearance.
Role: Behavioral Specialists (if applicable)
Requirements: Certification in behavioral analysis or related field; experience in therapeutic interventions; background clearance.
All staff must complete:
Training in client safety, personal care, and infection control
HIPAA compliance and participant rights education
Annual competency evaluations and ongoing professional development
Safety training, including emergency preparedness
7. MEDICAID WAIVER PROGRAMS
HCBS are available under the following New Jersey Medicaid Waivers:
Community Care Program for the Elderly and Disabled (CCPED)
Supports Program Waiver
Acquired Brain Injury (ABI) Waiver
Personal Care Assistant (PCA) Waiver
Home and Community-Based Services (HCBS) Waiver
Services may include:
In-home personal care and health monitoring
Community-based support and engagement activities
Skilled nursing and health-related services
Behavioral interventions and case management
Transportation and mobility support
8. TIMELINE TO LAUNCH
Phase: Business Formation and Compliance Preparation
Timeline: 1–2 months
Phase: Staff Hiring, Credentialing, and Program Development
Timeline: 2–3 months
Phase: New Jersey Medicaid Provider Enrollment and Readiness Review
Timeline: 60–90 days
Phase: Medicaid Billing Setup and HCBS Service Launch
Timeline: 30–45 days
9. CONTACT INFORMATION
New Jersey Department of Human Services (DHS)
Website: https://www.state.nj.us/humanservices/
Division of Aging Services (DoAS)
Website: https://www.state.nj.us/humanservices/doas/
Division of Developmental Disabilities (DDD)
Website: https://www.state.nj.us/humanservices/ddd/
New Jersey Medicaid Provider Enrollment Portal
Website: https://www.njmmis.com/
Centers for Medicare & Medicaid Services (CMS)
Website: https://www.cms.gov/
WAIVER CONSULTING GROUP’S START-UP ASSISTANCE SERVICE — NEW JERSEY IN-HOME AND COMMUNITY-BASED SERVICES PROVIDER
WCG supports agencies in launching Medicaid-compliant HCBS in New Jersey, offering:
Scope of Work:
Business registration, Medicaid enrollment, and licensing assistance
Policy manual development for care planning and safety management
Staff credentialing, training program templates, and compliance documentation
Medicaid billing setup and audit-prepared financial management
Branding, website development, and community engagement strategies
Quality assurance systems for care delivery and safety compliance
Collaboration with healthcare and community organizations for coordinated support

Homemaker
HOMEMAKER SERVICES PROVIDER IN NEW JERSEY
SUPPORTING INDEPENDENT LIVING THROUGH ESSENTIAL HOUSEHOLD ASSISTANCE
Homemaker Services in New Jersey support individuals with disabilities, chronic illnesses, or age-related conditions by providing assistance with essential household tasks. These services help maintain a clean, safe, and comfortable living environment while promoting independence. Homemaker Services are authorized under New Jersey Medicaid Home and Community-Based Services (HCBS) Waiver programs.
1. GOVERNING AGENCIES
Agency: New Jersey Department of Human Services (DHS)
Role: Administers Medicaid waiver funding for Homemaker Services and manages provider enrollment, service authorization, and reimbursement.
Agency: Division of Aging Services (DoAS)
Role: Ensures quality standards, service delivery, and compliance for Homemaker Services under HCBS waiver programs.
Agency: Centers for Medicare & Medicaid Services (CMS)
Role: Provides federal oversight ensuring Medicaid-funded Homemaker Services meet HCBS quality, person-centered planning, and participant protection standards.
2. HOMEMAKER SERVICES OVERVIEW
Homemaker Services provide non-medical support to individuals, helping them maintain a clean and safe living environment.
Approved providers may deliver:
Housekeeping: Light cleaning, dusting, vacuuming, and trash removal.
Laundry and Linen Care: Washing, drying, folding, and changing bed linens.
Meal Preparation: Cooking and meal planning based on dietary needs.
Grocery Shopping: Purchasing groceries and household essentials.
Home Safety Checks: Identifying and addressing potential hazards.
Organization Assistance: Helping to maintain a clutter-free and organized space.
Companionship: Providing social interaction while completing tasks.
Errands: Assisting with light shopping and pharmacy visits.
All services are delivered according to the Individualized Service Plan (ISP) to meet the participant’s household and safety needs.
3. LICENSING & PROVIDER APPROVAL REQUIREMENTS
Prerequisites:
Register the business entity with the New Jersey Division of Revenue and Enterprise Services.
Obtain EIN from the IRS and NPI (Type 2).
Enroll as a Medicaid Waiver Homemaker provider via the New Jersey Medicaid Provider Enrollment Portal.
Obtain any required licensure from DHS if applicable.
Maintain general liability and professional liability insurance.
Develop policies for household management, safety protocols, and staff training.
Ensure staff meet background checks, health screenings, and homemaking training requirements.
4. NEW JERSEY PROVIDER ENROLLMENT PROCESS
Initial Interest and Application:
Complete the Provider Enrollment Application through the New Jersey Medicaid Provider Enrollment Portal for Homemaker Services under HCBS waivers.
Application and Documentation Submission:
Submit Articles of Incorporation, proof of EIN/NPI, insurance certificates, staff qualifications, and policy manuals.
Program Readiness Review:
DHS and DoAS evaluate provider readiness, including safety protocols, staff qualifications, and homemaker procedures.
Approval & Medicaid Enrollment:
Upon approval, providers are authorized to bill Medicaid for Homemaker Services using designated billing codes.
5. REQUIRED DOCUMENTATION
Articles of Incorporation or Business License (New Jersey Division of Revenue)
IRS EIN confirmation
NPI confirmation
Proof of general and professional liability insurance
Homemaker Services Policy & Procedure Manual including:
Participant intake, assessment, and service planning procedures
Housekeeping, meal preparation, and personal environment maintenance protocols
Staff credentialing, background checks, and ongoing training records
Documentation standards for service tracking and Medicaid billing
HIPAA compliance, participant rights, and grievance handling
Safety protocols, emergency response, and infection control measures
Quality assurance and compliance monitoring
6. STAFFING REQUIREMENTS
Role: Homemaker Program Director
Requirements: Bachelor’s degree in human services, healthcare administration, or related field; supervisory experience preferred.
Role: Homemakers/Direct Support Workers
Requirements: High school diploma or GED; basic housekeeping and meal preparation skills; CPR/First Aid certification; background clearance.
Role: Personal Care Aides (if applicable)
Requirements: CPR/First Aid certification; experience in light personal care assistance; background clearance.
All staff must complete:
Homemaking and light caregiving training
Safety and infection control education
HIPAA compliance and client rights training
Annual competency evaluations and continuing education
Ongoing training in household safety and wellness monitoring
7. MEDICAID WAIVER PROGRAMS
Homemaker Services are available under the following New Jersey Medicaid Waivers:
Community Care Program for the Elderly and Disabled (CCPED)
Supports Program Waiver
Acquired Brain Injury (ABI) Waiver
Personal Care Assistant (PCA) Waiver
Home and Community-Based Services (HCBS) Waiver
Services may include:
Light housekeeping and laundry assistance
Meal preparation and dietary support
Grocery shopping and essential errands
Safety checks and home maintenance assistance
Social interaction and companionship
8. TIMELINE TO LAUNCH
Phase: Business Formation and Compliance Preparation
Timeline: 1–2 months
Phase: Staff Hiring, Credentialing, and Program Development
Timeline: 2–3 months
Phase: New Jersey Medicaid Provider Enrollment and Readiness Review
Timeline: 60–90 days
Phase: Medicaid Billing Setup and Homemaker Service Launch
Timeline: 30–45 days
9. CONTACT INFORMATION
New Jersey Department of Human Services (DHS)
Website: https://www.state.nj.us/humanservices/
Division of Aging Services (DoAS)
Website: https://www.state.nj.us/humanservices/doas/
New Jersey Medicaid Provider Enrollment Portal
Website: https://www.njmmis.com/
Centers for Medicare & Medicaid Services (CMS)
Website: https://www.cms.gov/
WAIVER CONSULTING GROUP’S START-UP ASSISTANCE SERVICE — NEW JERSEY HOMEMAKER SERVICES PROVIDER
WCG supports agencies in launching Medicaid-compliant Homemaker Services in New Jersey, offering:
Scope of Work:
Business registration, Medicaid enrollment, and licensing assistance
Policy manual development for homemaking support and household safety
Staff credentialing, training program templates, and service documentation guidance
Medicaid billing setup and audit-prepared financial management
Branding, website development, and community outreach strategies
Quality assurance systems for household safety and compliance monitoring
Networking with community-based organizations for referrals
Collaboration with healthcare providers for coordinated travel support

Case Management
CASE MANAGEMENT SERVICES PROVIDER IN NEW JERSEY
COORDINATING CARE AND SUPPORT THROUGH INDIVIDUALIZED CASE MANAGEMENT
Case Management Services in New Jersey support individuals with disabilities, chronic conditions, or long-term care needs by coordinating services, developing care plans, and facilitating access to resources. These services ensure that individuals receive comprehensive, person-centered care. Case Management Services are authorized under New Jersey Medicaid Home and Community-Based Services (HCBS) Waiver programs.
1. GOVERNING AGENCIES
Agency: New Jersey Department of Human Services (DHS)
Role: Administers Medicaid waiver funding for Case Management Services and manages provider enrollment, service authorization, and reimbursement.
Agency: Division of Developmental Disabilities (DDD)
Role: Ensures quality standards, service delivery, and compliance for Case Management Services under HCBS waiver programs.
Agency: Centers for Medicare & Medicaid Services (CMS)
Role: Provides federal oversight ensuring Medicaid-funded Case Management Services meet HCBS quality, person-centered planning, and participant protection standards.
2. CASE MANAGEMENT SERVICES OVERVIEW
Case Management Services coordinate and manage care to enhance an individual’s ability to live independently and safely within the community.
Approved providers may deliver:
Needs Assessment: Conducting comprehensive evaluations to identify care requirements.
Service Planning: Developing an Individualized Service Plan (ISP) tailored to each participant.
Care Coordination: Arranging healthcare, social, and community services.
Monitoring and Follow-Up: Regularly reviewing progress and updating care plans as needed.
Crisis Intervention: Providing support during emergencies and coordinating responses.
Resource Navigation: Assisting individuals in accessing community resources and financial support.
Advocacy: Supporting participants in obtaining necessary services and advocating for their rights.
All services are delivered according to the ISP to meet the unique needs and preferences of the participant.
3. LICENSING & PROVIDER APPROVAL REQUIREMENTS
Prerequisites:
Register the business entity with the New Jersey Division of Revenue and Enterprise Services.
Obtain EIN from the IRS and NPI (Type 2).
Enroll as a Medicaid Waiver Case Management provider via the New Jersey Medicaid Provider Enrollment Portal.
Obtain any necessary licensure for case management services from DHS if applicable.
Maintain general liability and professional liability insurance.
Develop policies for care coordination, crisis response, and documentation.
Ensure staff meet background checks, health screenings, and case management training requirements.
4. NEW JERSEY PROVIDER ENROLLMENT PROCESS
Initial Interest and Application:
Complete the Provider Enrollment Application through the New Jersey Medicaid Provider Enrollment Portal for Case Management Services under HCBS waivers.
Application and Documentation Submission:
Submit Articles of Incorporation, proof of EIN/NPI, insurance certificates, staff qualifications, and policy manuals.
Program Readiness Review:
DHS and DDD evaluate provider readiness, including staff qualifications, service planning protocols, and safety measures.
Approval & Medicaid Enrollment:
Upon approval, providers are authorized to bill Medicaid for Case Management Services using designated billing codes.
5. REQUIRED DOCUMENTATION
Articles of Incorporation or Business License (New Jersey Division of Revenue)
IRS EIN confirmation
NPI confirmation
Proof of general and professional liability insurance
Case Management Services Policy & Procedure Manual including:
Participant intake, needs assessment, and care planning procedures
Coordination of healthcare, social, and community-based services
Crisis intervention and emergency response protocols
Staff credentialing, background checks, and ongoing training records
HIPAA compliance, participant rights, and grievance handling
Documentation standards for service coordination and Medicaid billing
Quality assurance and compliance monitoring
6. STAFFING REQUIREMENTS
Role: Case Management Program Director
Requirements: Bachelor’s or Master’s degree in social work, human services, or healthcare; certification in case management preferred; supervisory experience.
Role: Case Managers
Requirements: Bachelor’s degree in social work, healthcare, or a related field; experience in care coordination and service planning; background clearance.
Role: Case Management Assistants
Requirements: High school diploma or GED; experience in administrative support and data entry; background clearance.
All staff must complete:
Training in person-centered planning and case management practices
HIPAA compliance and participant rights education
Crisis management and de-escalation techniques
Annual competency evaluations and continuing education
Ongoing training in service coordination and resource management
7. MEDICAID WAIVER PROGRAMS
Case Management Services are available under the following New Jersey Medicaid Waivers:
Community Care Program for the Elderly and Disabled (CCPED)
Supports Program Waiver
Acquired Brain Injury (ABI) Waiver
Personal Care Assistant (PCA) Waiver
Home and Community-Based Services (HCBS) Waiver
Services may include:
Coordinating healthcare and supportive services
Developing and monitoring Individualized Service Plans (ISPs)
Assisting with accessing community resources and financial aid
Crisis intervention and emergency coordination
Providing advocacy and support for participant needs
8. TIMELINE TO LAUNCH
Phase: Business Formation and Compliance Preparation
Timeline: 1–2 months
Phase: Staff Hiring, Credentialing, and Program Development
Timeline: 2–3 months
Phase: New Jersey Medicaid Provider Enrollment and Readiness Review
Timeline: 60–90 days
Phase: Medicaid Billing Setup and Case Management Service Launch
Timeline: 30–45 days
9. CONTACT INFORMATION
New Jersey Department of Human Services (DHS)
Website: https://www.state.nj.us/humanservices/
Division of Developmental Disabilities (DDD)
Website: https://www.state.nj.us/humanservices/ddd/
New Jersey Medicaid Provider Enrollment Portal
Website: https://www.njmmis.com/
Centers for Medicare & Medicaid Services (CMS)
Website: https://www.cms.gov/
WAIVER CONSULTING GROUP’S START-UP ASSISTANCE SERVICE — NEW JERSEY CASE MANAGEMENT SERVICES PROVIDER
WCG supports agencies in launching Medicaid-compliant Case Management Services in New Jersey, offering:
Scope of Work:
Business registration, Medicaid enrollment, and licensing support
Policy manual development for care coordination and crisis management
Staff credentialing, training program templates, and documentation guidance
Medicaid billing setup and audit-prepared financial management
Branding, website development, and client engagement strategies
Quality assurance systems for service coordination and compliance
Collaboration with healthcare and community organizations for resource sharing

Adult Health Transportation
TRANSPORTATION SERVICES PROVIDER IN NEW JERSEY
ENSURING ACCESS TO CARE AND COMMUNITY THROUGH SAFE, RELIABLE TRANSPORTATION
Transportation Services in New Jersey provide non-emergency medical and community transportation for individuals with disabilities, chronic conditions, or mobility challenges. These services facilitate access to medical appointments, social activities, work, and community resources, promoting independence and social inclusion. Transportation Services are authorized under New Jersey Medicaid Home and Community-Based Services (HCBS) Waiver programs.
1. GOVERNING AGENCIES
Agency: New Jersey Department of Human Services (DHS)
Role: Administers Medicaid waiver funding for Transportation Services and manages provider enrollment, service authorization, and reimbursement.
Agency: Division of Medical Assistance and Health Services (DMAHS)
Role: Ensures quality standards, service delivery, and compliance for Transportation Services under HCBS waiver programs.
Agency: Centers for Medicare & Medicaid Services (CMS)
Role: Provides federal oversight ensuring Medicaid-funded Transportation Services meet HCBS quality, person-centered planning, and participant protection standards.
2. TRANSPORTATION SERVICES OVERVIEW
Transportation Services ensure that individuals with disabilities have access to healthcare, social, and community activities through reliable transportation.
Approved providers may deliver:
Non-Emergency Medical Transportation (NEMT): Rides to medical appointments, therapies, and healthcare services.
Community Access Transportation: Travel to community centers, social events, and support groups.
Employment Transportation: Rides to work or vocational training.
Recreational and Social Transportation: Facilitating participation in community events and activities.
Specialized Transport: Vehicles equipped for wheelchairs, mobility aids, and accessible seating.
Door-to-Door Assistance: Helping passengers from their residence to the vehicle and destination.
Escort or Companion Services: Assisting individuals who need additional support during travel.
All services are delivered according to the Individualized Service Plan (ISP) to meet the specific transportation needs of the participant.
3. LICENSING & PROVIDER APPROVAL REQUIREMENTS
Prerequisites:
Register the business entity with the New Jersey Division of Revenue and Enterprise Services.
Obtain EIN from the IRS and NPI (Type 2).
Enroll as a Medicaid Waiver Transportation provider via the New Jersey Medicaid Provider Enrollment Portal.
Obtain necessary permits and licenses from the New Jersey Motor Vehicle Commission (MVC).
Maintain general liability, professional liability, and vehicle insurance.
Develop policies for passenger safety, vehicle maintenance, and driver training.
Ensure drivers meet background checks, health screenings, and defensive driving training requirements.
4. NEW JERSEY PROVIDER ENROLLMENT PROCESS
Initial Interest and Application:
Complete the Provider Enrollment Application through the New Jersey Medicaid Provider Enrollment Portal for Transportation Services under HCBS waivers.
Application and Documentation Submission:
Submit Articles of Incorporation, proof of EIN/NPI, vehicle insurance certificates, driver qualifications, and policy manuals.
Program Readiness Review:
DHS and DMAHS evaluate provider readiness, including safety protocols, driver training, and vehicle maintenance procedures.
Approval & Medicaid Enrollment:
Upon approval, providers are authorized to bill Medicaid for Transportation Services using designated billing codes.
5. REQUIRED DOCUMENTATION
Articles of Incorporation or Business License (New Jersey Division of Revenue)
IRS EIN confirmation
NPI confirmation
Vehicle Registration and Safety Inspection Documents
Proof of general liability, professional liability, and vehicle insurance
Transportation Services Policy & Procedure Manual including:
Trip scheduling, passenger assistance, and route planning procedures
Driver credentialing, background checks, and training records
Safety protocols for transporting individuals with mobility aids
Vehicle maintenance, inspection, and cleanliness standards
HIPAA compliance, passenger rights, and grievance handling
Documentation standards for trip logs, billing, and compliance tracking
Emergency preparedness, accident reporting, and incident management
6. STAFFING REQUIREMENTS
Role: Transportation Program Director
Requirements: Bachelor’s degree in business administration, transportation management, or related field; supervisory experience preferred.
Role: Drivers/Transportation Aides
Requirements: Valid New Jersey driver’s license with a clean driving record; defensive driving and passenger assistance training; CPR/First Aid certification; background clearance.
Role: Dispatch Coordinators
Requirements: Experience in logistics, scheduling, and customer support; background clearance.
All staff must complete:
Training in safe driving practices and passenger assistance
HIPAA compliance and client rights education
Ongoing professional development and defensive driving courses
Annual vehicle safety inspections and maintenance training
Customer service and accessibility training
7. MEDICAID WAIVER PROGRAMS
Transportation Services are available under the following New Jersey Medicaid Waivers:
Community Care Program for the Elderly and Disabled (CCPED)
Supports Program Waiver
Acquired Brain Injury (ABI) Waiver
Personal Care Assistant (PCA) Waiver
Home and Community-Based Services (HCBS) Waiver
Services may include:
Non-emergency medical transportation to healthcare facilities
Community access rides to social and recreational programs
Vocational transportation to work or training sites
Door-to-door assistance for individuals requiring mobility support
Specialized transport for individuals using wheelchairs or mobility aids
8. TIMELINE TO LAUNCH
Phase: Business Formation and Compliance Preparation
Timeline: 1–2 months
Phase: Staff Hiring, Credentialing, and Program Development
Timeline: 2–3 months
Phase: New Jersey Medicaid Provider Enrollment and Readiness Review
Timeline: 60–90 days
Phase: Medicaid Billing Setup and Transportation Service Launch
Timeline: 30–45 days
9. CONTACT INFORMATION
New Jersey Department of Human Services (DHS)
Website: https://www.state.nj.us/humanservices/
Division of Medical Assistance and Health Services (DMAHS)
Website: https://www.state.nj.us/humanservices/dmahs/
New Jersey Motor Vehicle Commission (MVC)
Website: https://www.state.nj.us/mvc/
New Jersey Medicaid Provider Enrollment Portal
Website: https://www.njmmis.com/
Centers for Medicare & Medicaid Services (CMS)
Website: https://www.cms.gov/
WAIVER CONSULTING GROUP’S START-UP ASSISTANCE SERVICE — NEW JERSEY TRANSPORTATION SERVICES PROVIDER
WCG supports agencies in launching Medicaid-compliant Transportation Services in New Jersey, offering:
Scope of Work:
Business registration, Medicaid enrollment, and licensing assistance
Policy manual development for safe transportation and client support
Staff credentialing, training program templates, and compliance documentation
Medicaid billing setup and audit-prepared financial management
Branding, website development, and community engagement strategies
Quality assurance systems for transportation safety and driver training
Collaboration with healthcare providers for coordinated travel support

Home Health
HOME HEALTH SERVICES PROVIDER IN NEW JERSEY
DELIVERING MEDICAL AND PERSONAL CARE IN THE COMFORT OF HOME
Home Health Services in New Jersey provide medical care, personal assistance, and therapeutic support for individuals with chronic conditions, disabilities, or age-related health needs. These services are delivered in the home, allowing individuals to receive high-quality care while maintaining independence. Home Health Services are authorized under New Jersey Medicaid Home and Community-Based Services (HCBS) Waiver programs.
1. GOVERNING AGENCIES
Agency: New Jersey Department of Human Services (DHS)
Role: Administers Medicaid waiver funding for Home Health Services and manages provider enrollment, service authorization, and reimbursement.
Agency: Division of Medical Assistance and Health Services (DMAHS)
Role: Oversees quality standards, service delivery, and compliance for Home Health Services under HCBS waiver programs.
Agency: Centers for Medicare & Medicaid Services (CMS)
Role: Provides federal oversight ensuring Medicaid-funded Home Health Services meet HCBS quality, person-centered planning, and participant protection standards.
2. HOME HEALTH SERVICES OVERVIEW
Home Health Services provide a combination of medical, personal, and supportive care delivered in the individual’s home to enhance quality of life and maintain independence.
Approved providers may deliver:
Skilled Nursing: Health assessments, wound care, medication management, and chronic disease monitoring.
Therapeutic Services: Physical, occupational, and speech therapy to improve mobility, function, and communication.
Personal Care Assistance: Support with bathing, grooming, dressing, and mobility.
Health Monitoring: Checking vital signs, glucose levels, and respiratory function.
Medication Administration: Administering oral, injectable, and IV medications as prescribed.
Post-Surgical Care: Monitoring recovery, pain management, and wound dressing changes.
Rehabilitation Support: Exercises and routines designed to restore physical function.
Patient and Family Education: Teaching care techniques and health management strategies.
Care Coordination: Collaborating with healthcare providers to ensure comprehensive care.
Emergency Response Planning: Preparing for health crises and establishing protocols.
All services are delivered according to the Individualized Service Plan (ISP) to meet the participant’s health and personal care needs.
3. LICENSING & PROVIDER APPROVAL REQUIREMENTS
Prerequisites:
Register the business entity with the New Jersey Division of Revenue and Enterprise Services.
Obtain EIN from the IRS and NPI (Type 2).
Enroll as a Medicaid Waiver Home Health provider via the New Jersey Medicaid Provider Enrollment Portal.
Obtain a Home Health Agency License from the New Jersey Department of Health (NJDOH).
Maintain general liability and professional liability insurance.
Develop policies for clinical care, medication management, and personal care assistance.
Ensure staff meet background checks, health screenings, and professional licensure requirements.
4. NEW JERSEY PROVIDER ENROLLMENT PROCESS
Initial Interest and Application:
Complete the Provider Enrollment Application through the New Jersey Medicaid Provider Enrollment Portal for Home Health Services under HCBS waivers.
Application and Documentation Submission:
Submit Articles of Incorporation, proof of EIN/NPI, home health agency licenses, insurance certificates, and policy manuals.
Program Readiness Review:
DHS and DMAHS evaluate provider readiness, including care protocols, staff qualifications, and safety measures.
Approval & Medicaid Enrollment:
Upon approval, providers are authorized to bill Medicaid for Home Health Services using designated billing codes.
5. REQUIRED DOCUMENTATION
Articles of Incorporation or Business License (New Jersey Division of Revenue)
IRS EIN confirmation
NPI confirmation
Home Health Agency License
Proof of general and professional liability insurance
Home Health Services Policy & Procedure Manual including:
Health assessment, care planning, and medication management protocols
Personal care and hygiene assistance guidelines
Staff credentialing, background checks, and ongoing training records
Documentation standards for clinical care tracking and Medicaid billing
HIPAA compliance, patient rights, and grievance handling
Safety protocols, emergency response, and infection control measures
Quality assurance and compliance monitoring
6. STAFFING REQUIREMENTS
Role: Home Health Program Director
Requirements: Bachelor’s or Master’s degree in nursing, healthcare administration, or related field; RN license preferred.
Role: Registered Nurses (RNs)
Requirements: Valid RN license in New Jersey; experience in home healthcare; CPR/First Aid certification; background clearance.
Role: Licensed Practical Nurses (LPNs)
Requirements: Valid LPN license in New Jersey; experience in skilled nursing care; background clearance.
Role: Home Health Aides (HHAs)
Requirements: Certified as a Home Health Aide; experience in personal care and ADL assistance; background clearance.
Role: Therapists (Physical, Occupational, Speech)
Requirements: State licensure; experience in therapeutic home care; background clearance.
All staff must complete:
Training in clinical protocols, medication administration, and infection control
HIPAA compliance and patient rights education
Ongoing professional development and certification renewal
Annual competency evaluations and safety protocol updates
CPR/First Aid and emergency response training
7. MEDICAID WAIVER PROGRAMS
Home Health Services are available under the following New Jersey Medicaid Waivers:
Community Care Program for the Elderly and Disabled (CCPED)
Supports Program Waiver
Acquired Brain Injury (ABI) Waiver
Personal Care Assistant (PCA) Waiver
Home and Community-Based Services (HCBS) Waiver
Services may include:
Health monitoring and chronic disease management
Medication administration and adherence support
Rehabilitation and therapeutic exercises
Personal care and hygiene assistance
Health education and wellness planning
8. TIMELINE TO LAUNCH
Phase: Business Formation and Compliance Preparation
Timeline: 1–2 months
Phase: Staff Hiring, Credentialing, and Program Development
Timeline: 2–3 months
Phase: New Jersey Medicaid Provider Enrollment and Readiness Review
Timeline: 60–90 days
Phase: Medicaid Billing Setup and Home Health Service Launch
Timeline: 30–45 days
9. CONTACT INFORMATION
New Jersey Department of Human Services (DHS)
Website: https://www.state.nj.us/humanservices/
Division of Medical Assistance and Health Services (DMAHS)
Website: https://www.state.nj.us/humanservices/dmahs/
New Jersey Department of Health (NJDOH)
Website: https://www.nj.gov/health/
New Jersey Medicaid Provider Enrollment Portal
Website: https://www.njmmis.com/
Centers for Medicare & Medicaid Services (CMS)
Website: https://www.cms.gov/
WAIVER CONSULTING GROUP’S START-UP ASSISTANCE SERVICE — NEW JERSEY HOME HEALTH SERVICES PROVIDER
WCG supports agencies in launching Medicaid-compliant Home Health Services in New Jersey, offering:
Scope of Work:
Business registration, Medicaid enrollment, and licensing assistance
Policy manual development for clinical care and patient safety
Staff credentialing, training program templates, and compliance documentation
Medicaid billing setup and audit-prepared financial management
Branding, website development, and client engagement strategies
Quality assurance systems for clinical care and compliance monitoring
Collaboration with healthcare providers and community organizations

Meal & Nutrition
MEAL AND NUTRITION SERVICES PROVIDER IN NEW JERSEY
PROMOTING HEALTH AND WELL-BEING THROUGH NUTRITIONAL SUPPORT
Meal and Nutrition Services in New Jersey provide essential nutritional support to individuals with disabilities, chronic conditions, or age-related dietary needs. These services help ensure that individuals receive balanced, healthy meals tailored to their preferences and medical requirements. Meal and Nutrition Services are authorized under New Jersey Medicaid Home and Community-Based Services (HCBS) Waiver programs.
1. GOVERNING AGENCIES
Agency: New Jersey Department of Human Services (DHS)
Role: Administers Medicaid waiver funding for Meal and Nutrition Services and manages provider enrollment, service authorization, and reimbursement.
Agency: Division of Aging Services (DoAS)
Role: Ensures quality standards, service delivery, and compliance for Meal and Nutrition Services under HCBS waiver programs.
Agency: Centers for Medicare & Medicaid Services (CMS)
Role: Provides federal oversight ensuring Medicaid-funded Meal and Nutrition Services meet HCBS quality, person-centered planning, and participant protection standards.
2. MEAL AND NUTRITION SERVICES OVERVIEW
Meal and Nutrition Services support individuals by offering prepared meals, meal planning, and dietary guidance to maintain health and well-being.
Approved providers may deliver:
Meal Preparation: Cooking and delivering nutritious meals based on individual dietary needs.
Meal Planning: Developing customized meal plans tailored to health conditions (e.g., diabetes, hypertension).
Nutritional Counseling: Guidance on maintaining a balanced diet.
Specialized Diets: Preparing meals that accommodate medical conditions (e.g., low-sodium, pureed, or allergen-free diets).
Home-Delivered Meals: Regular meal delivery for those unable to prepare food themselves.
On-Site Congregate Meals: Group meal settings for social engagement and community interaction.
Dietary Monitoring: Tracking dietary intake and ensuring nutritional adequacy.
Food Safety and Hygiene: Ensuring that meals are prepared and stored safely.
All services are delivered according to the Individualized Service Plan (ISP) to meet the participant’s dietary and health needs.
3. LICENSING & PROVIDER APPROVAL REQUIREMENTS
Prerequisites:
Register the business entity with the New Jersey Division of Revenue and Enterprise Services.
Obtain EIN from the IRS and NPI (Type 2).
Enroll as a Medicaid Waiver Meal and Nutrition provider via the New Jersey Medicaid Provider Enrollment Portal.
Obtain a food establishment license from the New Jersey Department of Health (NJDOH).
Maintain general liability and professional liability insurance.
Develop policies for meal preparation, dietary planning, and food safety.
Ensure staff meet background checks, health screenings, and food safety training requirements.
4. NEW JERSEY PROVIDER ENROLLMENT PROCESS
Initial Interest and Application:
Complete the Provider Enrollment Application through the New Jersey Medicaid Provider Enrollment Portal for Meal and Nutrition Services under HCBS waivers.
Application and Documentation Submission:
Submit Articles of Incorporation, proof of EIN/NPI, food establishment license, insurance certificates, and policy manuals.
Program Readiness Review:
DHS and DoAS evaluate provider readiness, including meal planning protocols, safety measures, and staff qualifications.
Approval & Medicaid Enrollment:
Upon approval, providers are authorized to bill Medicaid for Meal and Nutrition Services using designated billing codes.
5. REQUIRED DOCUMENTATION
Articles of Incorporation or Business License (New Jersey Division of Revenue)
IRS EIN confirmation
NPI confirmation
Food Establishment License (if applicable)
Proof of general and professional liability insurance
Meal and Nutrition Services Policy & Procedure Manual including:
Meal preparation, dietary planning, and food safety protocols
Staff credentialing, background checks, and food handler certifications
Documentation standards for meal tracking and Medicaid billing
HIPAA compliance, participant rights, and grievance handling
Safety protocols for food storage, preparation, and delivery
Nutritional assessment and monitoring procedures
Quality assurance and compliance monitoring
6. STAFFING REQUIREMENTS
Role: Meal and Nutrition Program Director
Requirements: Bachelor’s degree in nutrition, dietetics, or food service management; supervisory experience preferred.
Role: Dietitians/Nutritionists
Requirements: Licensed or registered dietitian; experience in meal planning and dietary counseling; background clearance.
Role: Food Service Workers
Requirements: High school diploma or GED; food safety certification (e.g., ServSafe); background clearance.
Role: Delivery Personnel
Requirements: Valid driver’s license; background clearance; training in food safety and delivery protocols.
All staff must complete:
Food safety and hygiene training
HIPAA compliance and participant rights education
Ongoing professional development in dietary management
Annual competency evaluations and food safety refresher courses
Training in dietary monitoring and nutrition tracking
7. MEDICAID WAIVER PROGRAMS
Meal and Nutrition Services are available under the following New Jersey Medicaid Waivers:
Community Care Program for the Elderly and Disabled (CCPED)
Supports Program Waiver
Acquired Brain Injury (ABI) Waiver
Personal Care Assistant (PCA) Waiver
Home and Community-Based Services (HCBS) Waiver
Services may include:
Home-delivered meals for individuals with mobility or health challenges
Nutritional counseling for maintaining balanced diets
Specialized diet planning for chronic conditions
Group meal programs for social engagement
Regular dietary monitoring and health tracking
8. TIMELINE TO LAUNCH
Phase: Business Formation and Compliance Preparation
Timeline: 1–2 months
Phase: Staff Hiring, Credentialing, and Program Development
Timeline: 2–3 months
Phase: New Jersey Medicaid Provider Enrollment and Readiness Review
Timeline: 60–90 days
Phase: Medicaid Billing Setup and Meal and Nutrition Service Launch
Timeline: 30–45 days
9. CONTACT INFORMATION
New Jersey Department of Human Services (DHS)
Website: https://www.state.nj.us/humanservices/
Division of Aging Services (DoAS)
Website: https://www.state.nj.us/humanservices/doas/
New Jersey Department of Health (NJDOH)
Website: https://www.nj.gov/health/
New Jersey Medicaid Provider Enrollment Portal
Website: https://www.njmmis.com/
Centers for Medicare & Medicaid Services (CMS)
Website: https://www.cms.gov/
WAIVER CONSULTING GROUP’S START-UP ASSISTANCE SERVICE — NEW JERSEY MEAL AND NUTRITION SERVICES PROVIDER
WCG supports agencies in launching Medicaid-compliant Meal and Nutrition Services in New Jersey, offering:
Scope of Work:
Business registration, Medicaid enrollment, and food service licensing assistance
Policy manual development for meal preparation, dietary planning, and safety management
Staff credentialing, training program templates, and compliance documentation
Medicaid billing setup and audit-prepared financial management
Branding, website development, and community outreach strategies
Quality assurance systems for meal safety and dietary compliance
Collaboration with healthcare providers and nutrition experts

Our Client Portal offers a wealth of resources that you can explore related to various programs and state requirements.